It’s been a day and a half since Evan’s pacemaker was put in and he’s doing fairly well. A doctor came by this morning and “plugged into” the pacemaker to check everything out and said it was working great. There is a sensor that you hold up to the skin near the pacemaker and it communicates with the pacemaker. They are able to run diagnostics, change settings, and do all kinds of other things that I know nothing about. Once we go home we will have regular pacemaker checkups performed over the phone by holding a telephone up to the pacemaker and it will talk to a computer on the other end. Cool. I talked to him a little more about the decision to use a single chamber pacemaker instead of the dual since I was still grey on this. There were several reasons but the one that sticks in my head is that Evan is going to have at least two more surgeries and during those the surgeons will be working on and around the atrium. If they were to place the atrium leads now there is a chance that they would need to be moved or replaced during subsequent surgeries. When a lead is placed careful attention is payed to how well it’s conducting to the heart, scar tissue from moving the lead can reduce the conductivity of the heart tissues and make finding an optimal place for the lead more difficult. It’s not optimal that the atrium and ventricle are not firing synchronously and will eventually be corrected with a dual chamber pacemaker but with a baby this is much less of an issue… he’s not going to be running any marathons anytime soon.
Pretty normal things going on today for after surgery recovery… blood pressure stabilization, fluid retention, pain management, etc. He is still on the ventilator and they have been weaning him off throughout the day; the settings are currently as low as they go. Tonight they will do ‘sprints’ with him which are one hour blocks where they turn the ventilator down all the way and monitor his own breathing and how well his body is using the oxygen through blood tests and other monitoring. If that goes well then he’ll come off of the vent tomorrow. His blood pressure was a little iffy so they gave him some meds for that and that has since stabilized and the meds stopped. He’s on constant morphine for pain and gets an ‘extra’ dose when he looks particularly uncomfortable, like bath time. Last night when I was here the nurse had to suction the fluids out of his throat, something done quite often, but for some reason he was not happy about it. Instantly you could see on the monitor his blood pressure and heart rate shoot up and the looks on his face screamed “ouch.” The nurse was great she stopped what she was doing and went for the morphine, within a minute or two he had calmed down. It’s such a hard thing to see your child in such pain and be able to do nothing more than to caress their head and whisper into their ear, which I am sure does very little for them and more for me.
One potential issue today… a fever. We came back from dinner and the nurse said he was at 102°F. He was pretty bundled up and it is very warm in here for some reason. They immediately put him on antibiotics (vancomycin, which is pretty much the end all be all of antibiotics) and took samples. It will be 2 days before the results come back since the cultures need time to grow. In the meantime they will treat him as though he does have something. If it turns out to be nothing great, but if it is something then they are 2 days ahead of it with antibiotics. His temperature was down to 97.9 the last time we checked so it might have been nothing at all. We’ll wait and see. It’s these kinds of things that you see a lot here that can be difficult. It seems that many of the heart kids are here not just here for heart problems but they have something else happen while they are here or when they go home that brings them back. Infections, viruses, etc. We’ve seen kids with MRSA, kids with stomach and intestine problems, etc, etc. One very sad story is of a girl named Eva that we were next to in the ICU. She was born in May, cleft lip and palate, premature, and a heart condition. She was too small to undergo the full Norwood operation and so underwent a hybrid operation to hold her over until she got bigger. She spent the next several weeks in the ICU fighting viral infections where she could not eat anything for 2 weeks while it ran its course. She had 3-4 of these infections, that’s 6-8 weeks without food in total, and 6-8 weeks of not growing. She was on IV nutrition, but that’s not going to help you grow. Her parents live 75 miles from here and took turns being with her, dad after work every night and mom all weekend, they also have a 2 year old at home. On July 28, the same day that we were kissing Evan goodbye for his big surgery, little Eva died of complications to a heart catheterization procedure. Sarah and I just found out about this the day before Evan’s pacemaker surgery and it hit us pretty hard. My heart goes out to the parents of the little ones that are not as fortunate as we have been.
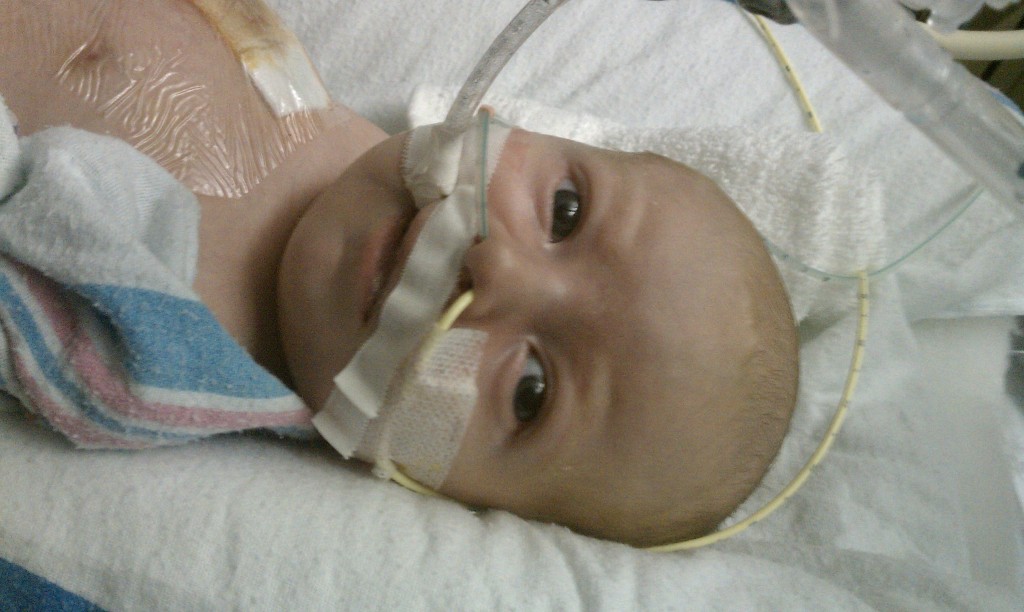
Evan opened his eyes nice and wide for the first time after surgery tonight… was great to see those beautiful eyes. He looked around for a little bit and we had a good conversation about how well he was doing and to keep it up. Then he got bored and fell back to sleep.
I’ve also updated the Treatment of TA/l-TGA page with more detailed information of what was performed during the first surgery if you are interested.
Leave a Reply