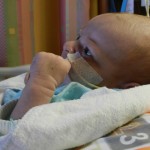
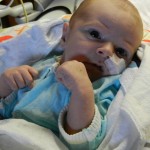
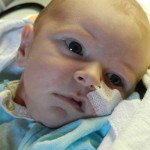
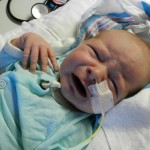
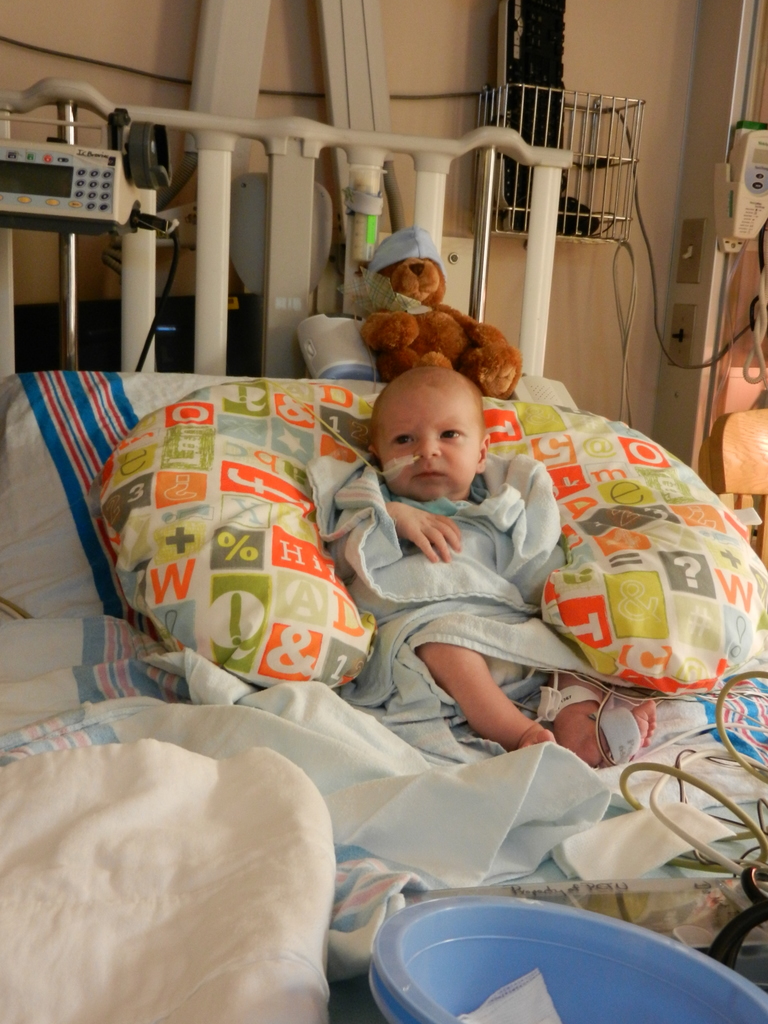
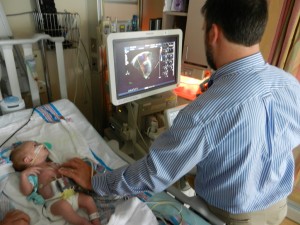
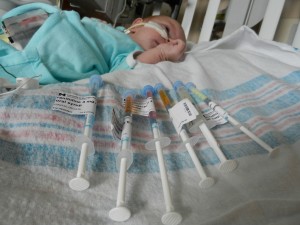
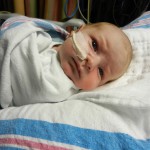
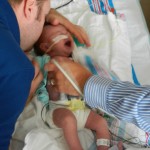
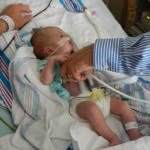
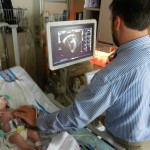
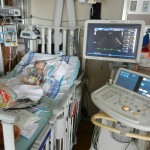
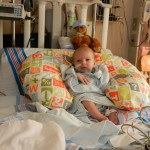
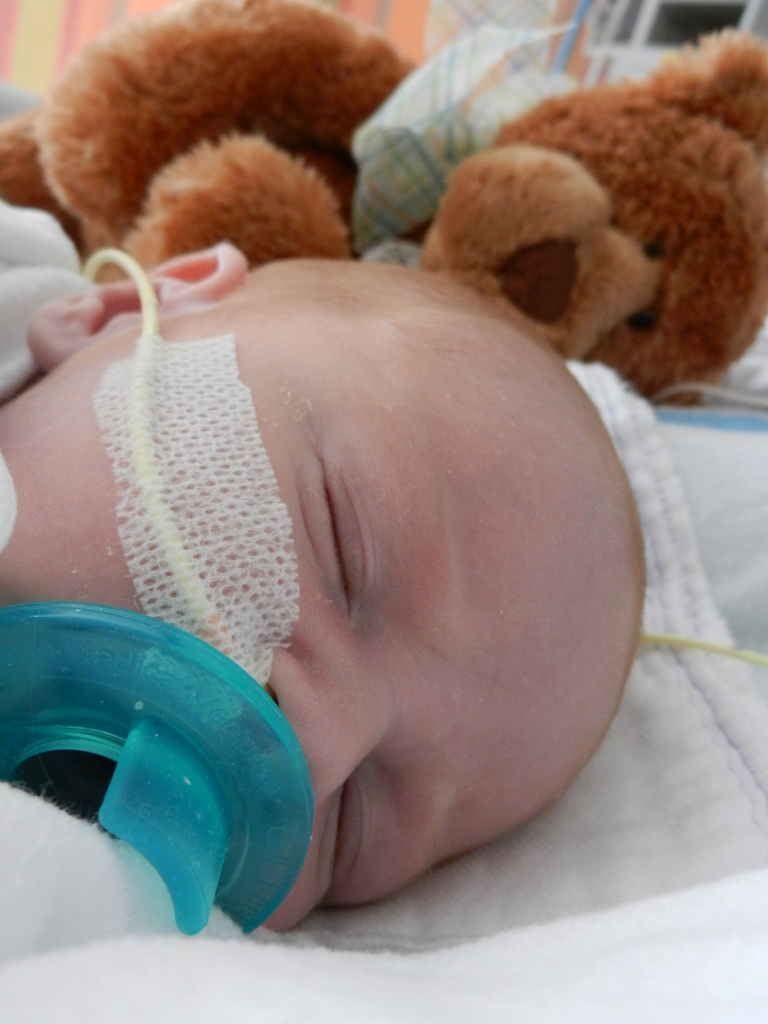
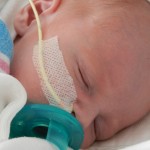
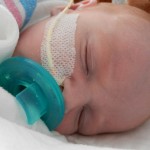
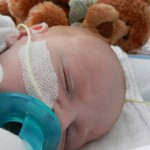
I mentioned in yesterday’s post that his surgery was scheduled for 11:30AM today. The surgeon performing the operation is still working on the 1st case of the day so ours is being delayed. Sarah and I are hanging out with Evan waiting to hear when they are going to take him down. Evan has not had any food since 8AM and considering he usually eats every 3 hours he’s doing really, really well. He’s very awake but he’s not fussy and he is sucking away on his pacifier which he doesn’t usually do. Hopefully the surgeons call him down before he realizes that the pacifier isn’t filling up his belly and he starts wailing.
I was surprised last night when I realized that I am just as nervous (or maybe even more) for this surgery than I was for the last one. It’s much, much less invasive, he does not need to go on a bypass machine, they don’t need to cut open his heart yet I am feeling the same things that I did on the morning of the first surgery. I left the hospital and went to see a movie to occupy my thoughts. After the movie however, I could not even think about going to sleep, I went back to the hotel, showered, changed my clothes, and spent the rest of the night back at the hospital. It’s quite a different place at 2AM, you should see the awesome parking spot that I got. 🙂
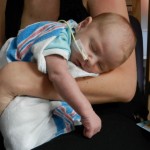
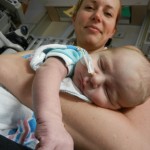
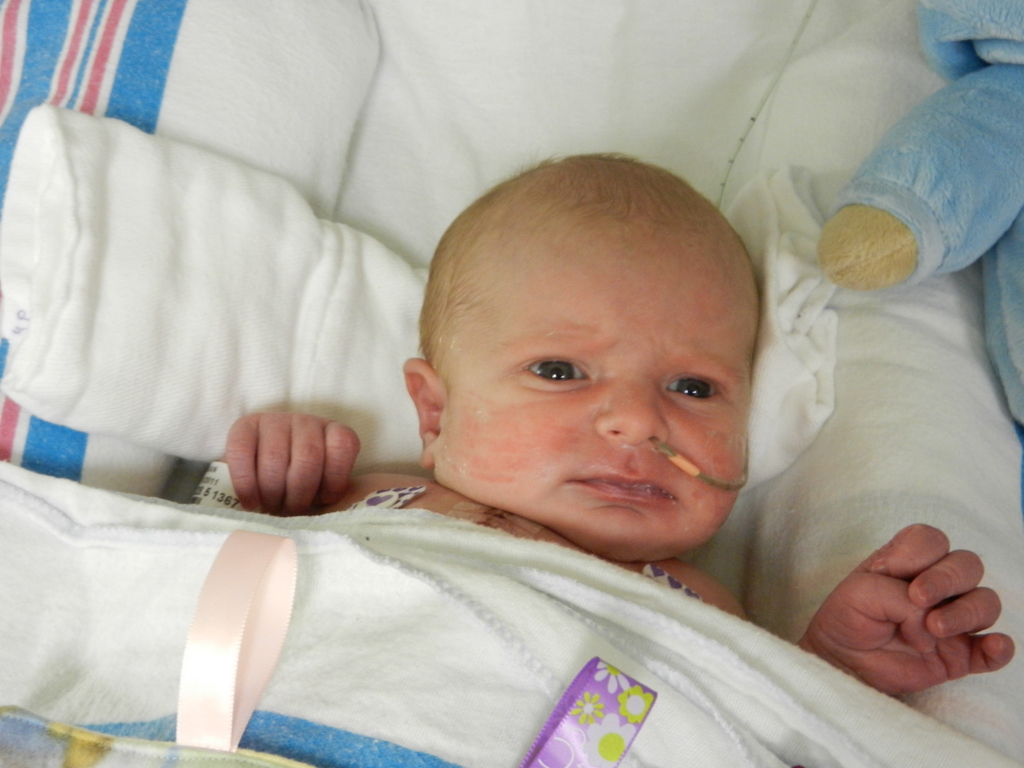
It’s been 3 weeks now with the little guy and I know him that much better than I did two weeks ago. I see pieces of his personality, I am beginning to learn his cries and things that work for consoling him, which lucky for us, is almost anything. He has been such a great baby. Of course he cries but it’s short lived and usually pretty obvious what the problem is… first I look at my watch, how long has it been since his last feeding? 3 hours? OK, he’s hungry. Not been 3 hours yet? Well he probably needs a diaper change. Only on a handful of occasions has it gone any further than that. I know, I know, it’s still way to early to count my chickens, but let me live in this dream where he’s easy for a little bit longer. DOH! Jinxed myself…. unconsolable crying in full effect, but he’s hungry and can’t eat before surgery, that doesn’t count.
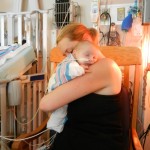
More updates later…. going to hold screaming baby now. 🙂