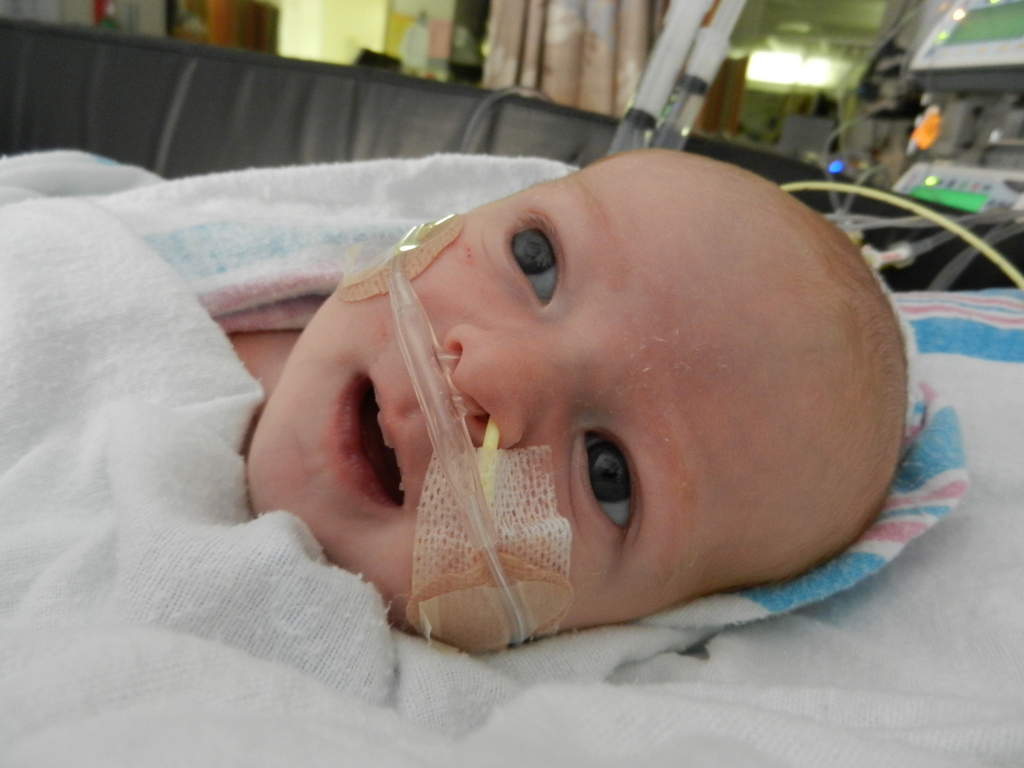
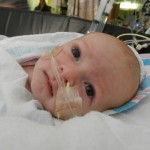
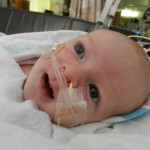
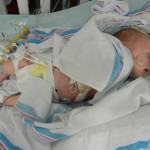
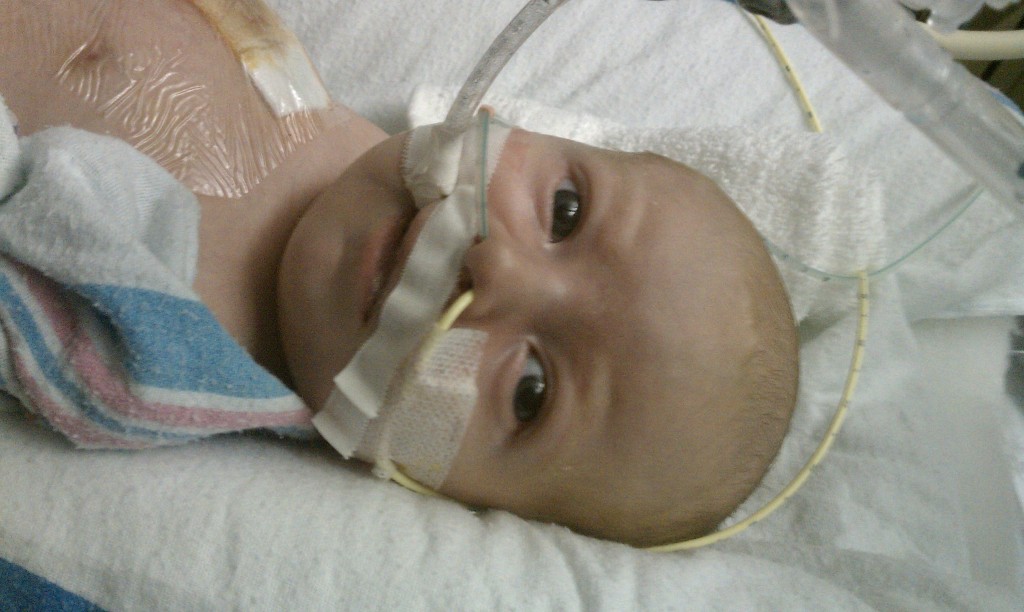
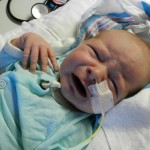
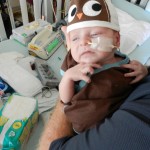
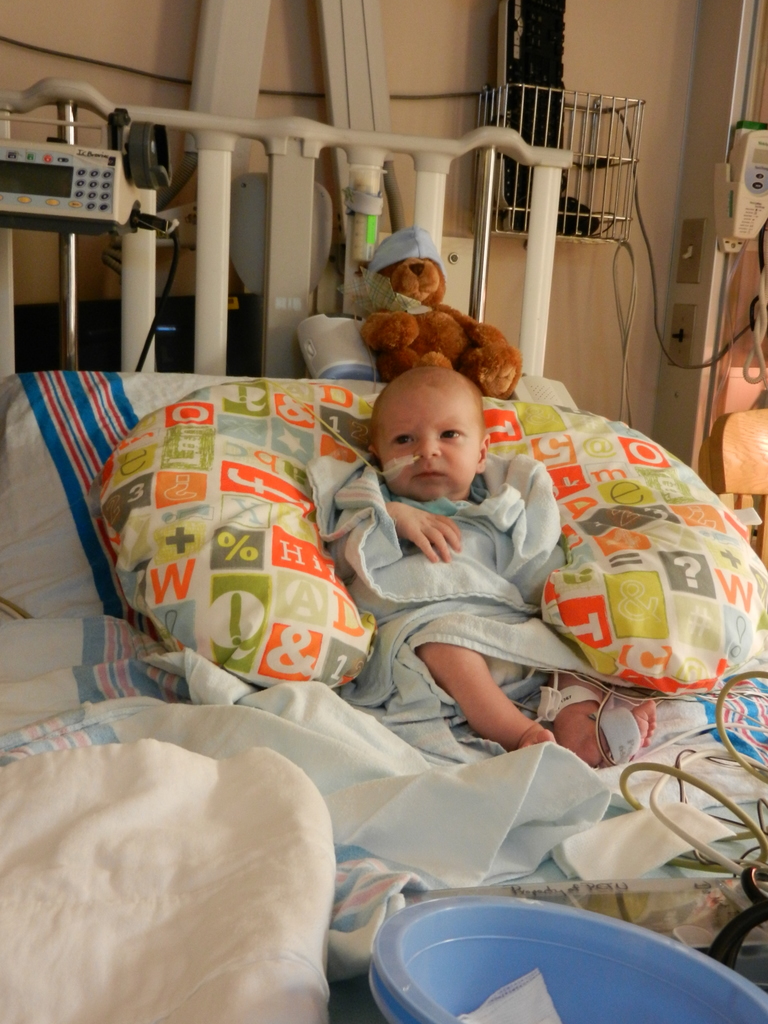
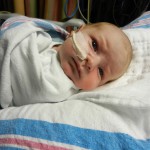
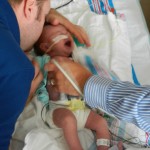
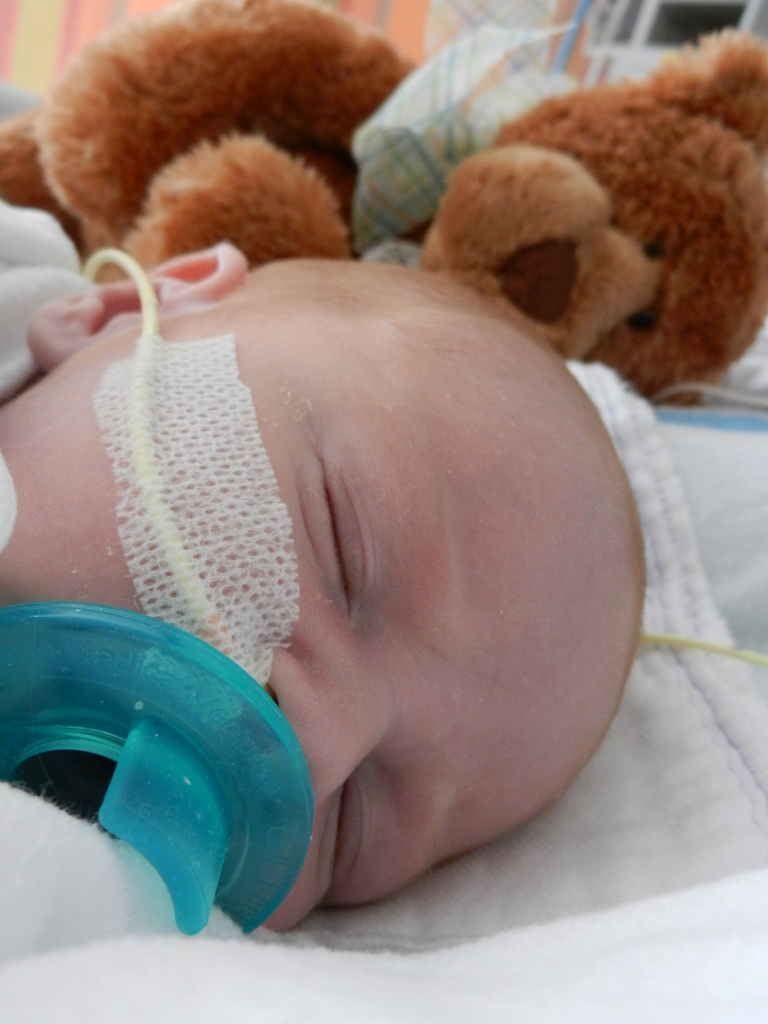
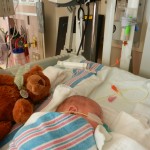
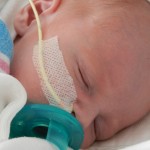
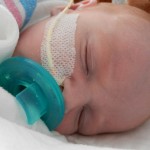
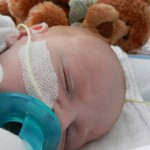
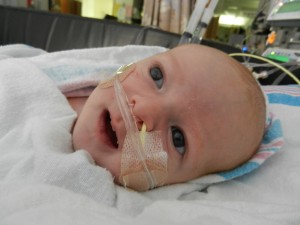
 A little bit of catch up is in order… my apologies. Yesterday Evan came off of the ventilator around noon. He had completed his sprints beautifully and came off it without any problems. He thrashed around a little bit so the nurses gave him some dexamethasone to reduce some swelling in his throat. He was still in some discomfort and once again had his little squeaky cry back but honestly sounded and looked better than the first time off the vent. Well, except for the coughing. His lung x-ray looked clear but he still has a lot of congestion in his chest and does his best to cough but he is obviously a little tender. The nurse tries to suction him, which of course is the equivalent of baby torture, but nothing much comes up. It must just be out of reach. He sounds much worse than he really is and with his solid coughing he should clear it up in a couple days.
A little bit of catch up is in order… my apologies. Yesterday Evan came off of the ventilator around noon. He had completed his sprints beautifully and came off it without any problems. He thrashed around a little bit so the nurses gave him some dexamethasone to reduce some swelling in his throat. He was still in some discomfort and once again had his little squeaky cry back but honestly sounded and looked better than the first time off the vent. Well, except for the coughing. His lung x-ray looked clear but he still has a lot of congestion in his chest and does his best to cough but he is obviously a little tender. The nurse tries to suction him, which of course is the equivalent of baby torture, but nothing much comes up. It must just be out of reach. He sounds much worse than he really is and with his solid coughing he should clear it up in a couple days.
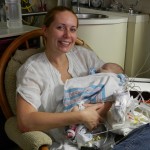
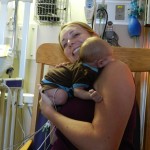
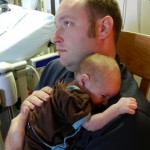
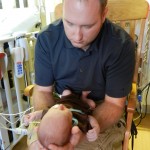
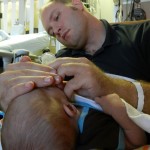
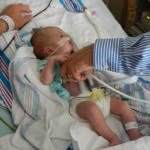
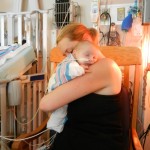
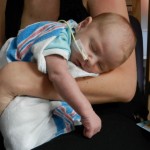
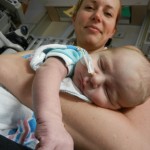
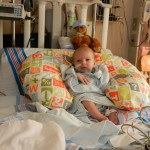
After coming off the vent the nurses like to wait 6 hours before resuming feeding. Because he is awesome and because he was going to have breastmilk, they let him start eating a little earlier and Evan was very happy about this. They start off on little increments and he chows it down like a champ. Hope fully he will be able to bounce back with eating better this time around than the first. But the best thing about coming off the vent is being able to hold the baby! We got our snuggles in for a few hours and the whole fam benefited greatly from this. You don’t know how much you miss something until you can’t do it anymore, that’s for sure. Although he was no longer on the vent and had significantly gone down on medications and support, they like to keep babies overnight in the PCTU for observation
This morning, Evan came off of Diurel and his arterial line was taken out. We moved from the PCTU down to general care around Noon! YAY! This should be our last stopbefore leaving the hospital. He still has his double lumen intracardiac broviac and an IV in his left hand. They will need to sedate him to remove the broviac so they are leaving the peripheral IV in for that purpose. His feeds are continuing to increase. Evan seems to have topped out at 20 ml but he has gone from 41 to 52 ml this evening and doesn’t continue to take more orally. The rest goes down his tube and it looks like we’ll have to work on this issue at home. Although he isn’t increasing in his oral intake we are very proud of his progress and it appears he is recovering from the vent much quicker this time around.
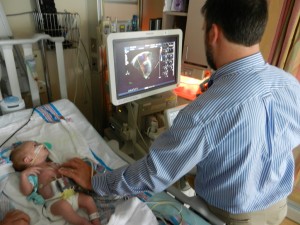
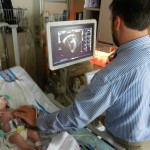
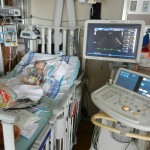
 There was some concern about fluid retention and the nurses are working at finding the right balance of medications and dosing. There was also some concern about fluid around Evan’s heart so an ultrasound was done by Dr. Mackie. I honestly don’t see how he can understand anything from the horribly grainy images, but his conclusion is that although there is some fluid around his heart it is not enough to worry about or drain. We were also able to take a small walk around the hospital floor this afternoon. Because Evan isn’t in a room with 24-hour nursing staff present he has to wear a tracking bracelet so he doesn’t get stolen. Our walk was limited to the areas not in front of elevators or down hallways. We are hoping that tomorrow we can go for a real walk and – gasp – maybe even venture outside! They are able to disable his house arrest bracelet for a set amount of time and we can certainly walk around the hospital. Outside might be pushing it but it will happen this week I’m sure. I now predict that we will be discharged on Thursday, unless there are issues scheduling his broviac removal and “little man” procedure. Then it would be Friday, but this week nonetheless. And we’d still meet our goal of leaving before he is 1 month old.
There was some concern about fluid retention and the nurses are working at finding the right balance of medications and dosing. There was also some concern about fluid around Evan’s heart so an ultrasound was done by Dr. Mackie. I honestly don’t see how he can understand anything from the horribly grainy images, but his conclusion is that although there is some fluid around his heart it is not enough to worry about or drain. We were also able to take a small walk around the hospital floor this afternoon. Because Evan isn’t in a room with 24-hour nursing staff present he has to wear a tracking bracelet so he doesn’t get stolen. Our walk was limited to the areas not in front of elevators or down hallways. We are hoping that tomorrow we can go for a real walk and – gasp – maybe even venture outside! They are able to disable his house arrest bracelet for a set amount of time and we can certainly walk around the hospital. Outside might be pushing it but it will happen this week I’m sure. I now predict that we will be discharged on Thursday, unless there are issues scheduling his broviac removal and “little man” procedure. Then it would be Friday, but this week nonetheless. And we’d still meet our goal of leaving before he is 1 month old.
Go Evan Go!