Nearly everyone remembers where they were on September 11, 2001. I was at work, at a graphic design company, my mom called to tell me that a plane had just hit one of the twin towers, the office was in shock. How many of you will remember where you were on September 11, 2014? I know that I will… September 11, 2014 was the day that my son had the last of three necessary open heart surgeries to make his brave little heart work the best that it possibly can. The end of a very long and difficult journey for him, Sarah, me, and all of the wonderful friends and family that have helped us along the way.
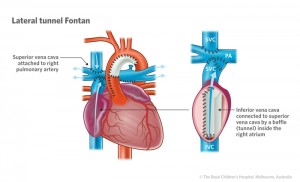
Dr. Romano came to give us the good news, Evan did great during surgery! The scar tissue was not nearly as bad as she was expecting so she was able to get into his chest without too much trouble. She completed the lateral tunnel Fontan procedure which uses a Gore-Tex tube to redirect bloodflow returning to the heart directly to the lungs (click on the image below to see a larger version). Additionally, based on Evan’s latest echo and heart catheterization the team also decided that they needed to place an additional pacemaker lead to improve his heart rhythm. This required a new incision and a new pacemaker with room for a third lead. So far the team is really happy with the new lead placement and how it has improved each beat.
It took about an hour and a half for them to get Evan up to his room, settled, and to let us come back. More great news is that he was breathing just fine on his own so he was extubated before he was even brought to the ICU. He’s very tired and mostly in a bad mood, who can blame him? He came up to the room on about 5 medications for pain, blood pressure, etc. His blood pressure looks great, so I expect that those will be discontinued by morning. They are going to start cutting back on some of the stronger IV pain medication and supplementing with some others that are able to be administered orally or on the general care floor.
Evan still has a long way to go, he has 3 chest tubes for drainage, a line in his foot, wrist, and neck for medications but he’s well on his way.
Thank you for all your kind words, encouragement, and support over the past few years. The outpouring of support has been nothing less than absolutely amazing and we’ll be forever grateful for it. Don’t stop! We’re not out of the hospital yet. 🙂 If you could also cast your net of support over a couple other families that are close to our hearts right now. Brittney is a high school student that had a heart transplant in 2008. Her heart is failing again and she has found herself back on the transplant list. 🙁 The second is a 5 month old baby named Charlie. Charlie has spent his entire life (aside from about 12 hours) in the hospital due primarily to a heart defect called Total Anomalous Pulmonary Venous Return. Both of these wonderful and dedicated families could use your thoughts and prayers.
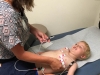
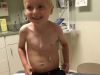
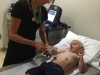
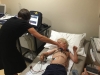
Here are a handful of pictures of Evan throughout his September 11th.
 Please consider joining Team Evan for the SW Michigan Congenital Heart Walk!
Please consider joining Team Evan for the SW Michigan Congenital Heart Walk!