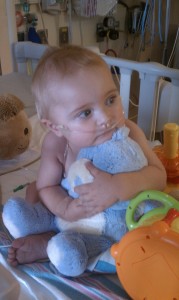
I cannot begin to put into words how grateful we are to have so many blessings. People may look at our life and take such pity or call us brave, but really we have so much to be thankful for. This is our version of normal so it really isn’t as overwhelming or cumbersome as you may think. Exhausting at times, emotionally draining at others… busy… but mostly happy, loved, and a work in progress. Evan has done so well despite his parents (ha) and their first-time-ed-ness.
The absolute truth is though that we wouldn’t be the people we are or in the place we are at if it wasn’t for an amazing network of support.
For my Raw Material Lab family, I am constantly blown away by your earnest care and consideration of my little man. Your genuine desire for him to do well and for me to keep some level of sanity are saint-worthy attributes. Your generous donations are more than I could have imagined. Forgoing your own individual rewards in order to give us gas cards may have been an easy decision for you to come to, but you deserved the reward as well. How many SQC hours can you log for Acts of Kindness? I will have to treat you to an off-site “research study” into the various forms of Ethanol. I owe you.
Karen and Nancy, you allowed me to leave work early the day before Evan’s surgery, which allowed me to have some cuddle time with my baby. Otherwise I would have gotten here too late and he would have been asleep. A mommy’s heart is so grateful for your unselfishness.
My other lab families, thank you for helping me find work that I can do while using my last 2 remaining brain cells. I don’t mind the grunt work. Thank you for not assigning me assays that require a 4-leaf clover and a lucky horseshoe to complete. I appreciate your patience. I won’t take the easy stuff forever. Thank you for the lunch dates. Your company is all I truly need.
For Bill’s Tech Transfer, ESTL, RTL, QA, and families, you are all so generous it is bordering on ridiculousness. You all are crazy. And thoughtful. And lovely. Would you accept a lunch date full of infant handsomeness as a sufficient thank-you? The best I can offer is for you to see the goodness that you helped to support.
For our bosses, our bosses’ boss, our bosses’ bosses’ boss…. Thank you for the sympathies, understanding, and flexibility. Everyone should be so fortunate to work with such wonderful people as we do.
Brittney, thank you for being so thoughtful and treating a hungry daddy to his favorite food.
Thank you to the Butcher family for both bringing our U of M Zipper Club shirts to the hospital and for the wonderful wooden puzzles.
Thank you to Scott Newport for the wonderful stool made from reclaimed wood and the redwood “tags,” we’ll put them to good use.
Carie and Jason, thank you for being constantly willing to open your house up to our barking, stinky, rambunctious dogs without complaint. We know they are well in your care and we know they drive you nuts. Your patience, friendship, and kindness are remarkable.
Kelly and Andrew, thank you for stepping in and filling in the holes with dog care despite the fact you have itty bitty twin girls and are (probably) slowly losing your sanity. Hey, maybe that’s why you keep offering…
To our fantastic chefs, homecooked meals do so much for the soul. Whether it is feeding us in the hospital or making sure we are taken care of once we go home. Relieving that from our minds was so wonderful:
- McLaren Family Sloppy Joes (delish and lasted several days)
- Erica’s Ravioli Lasagna (great, simple, yummy, easy!)
- Karen’s Homemade Pot Pie and Tofu Lasagna (first time trying parsnips, yum)
- Tracy and Executive Chef Bobby’s Homemade Soup (flavor perfection)
- Spilson Family Tacos (complete with baggies of toppings – so thoughtful) and Lasagna (perfect… and garlic bread to boot)
We aren’t brave or anything remarkable – this was our chosen path with a child we think was perfectly made. But your helping hands have absolutely made this journey much more manageable.
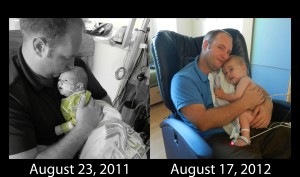
In todays picture album you will see visits from Bill’s parents and nephew Xander, physical therapy specialist Alaina, Cortney and Ian for a baby playdate, Sarah’s Mom and brother PJ and more cute pictures of Evan than you can handle. 🙂














































































































![[Yawn] Not much going on.](https://livingwithevan.com/wp-content/uploads/2012/08/DSCN8645-001.jpg)