10 days. No post in 10 days means good news for Evan. But no post in 10 days also means a bunch of well-intentioned individuals need their baby Evan fix. I apologize for that. The post delay is my fault. Seems to be that having a baby makes you the busiest you have ever been. It’s all I can do to keep up with a calendar for all of Evan’s events. And it’s all we can do to keep up with photos and videos, so they are a little bit more scarce as we aren’t always as camera ready as we were before.
Since the last post Grandma Nancee (my mom) came down and spent a few days with us. Unfortunately zero photographic evidence of this exists, but it was a lovely time. She was very useful in helping us get organized, putting things away, cooking, cleaning, gardening, and of course watching after the little man. I honestly don’t know how couples manage by themselves (I mean without extended family help). One fortunate thing throughout all of this is that I am healed, am physically able, and we were able to learn a bit about Evan’s personality and his routine before coming home. I can’t imagine having other kids at home and/or coming home with a 2 day old baby.
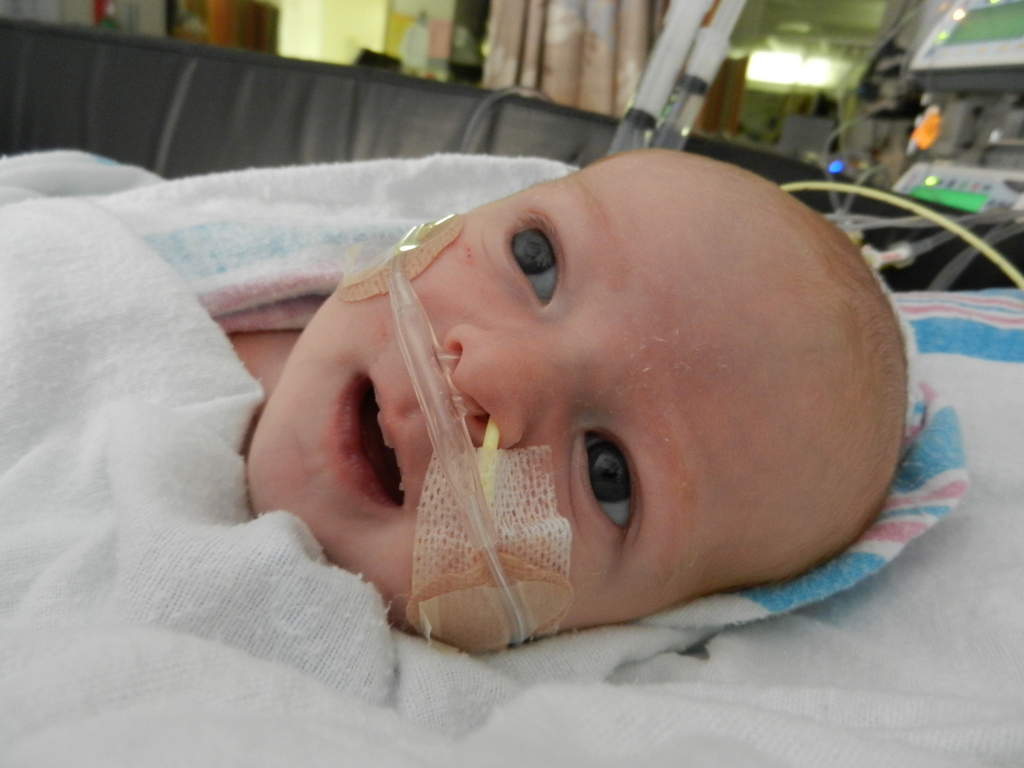
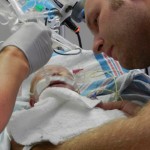
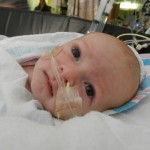
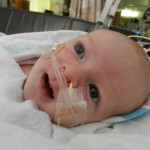
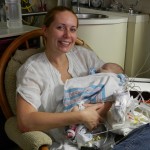
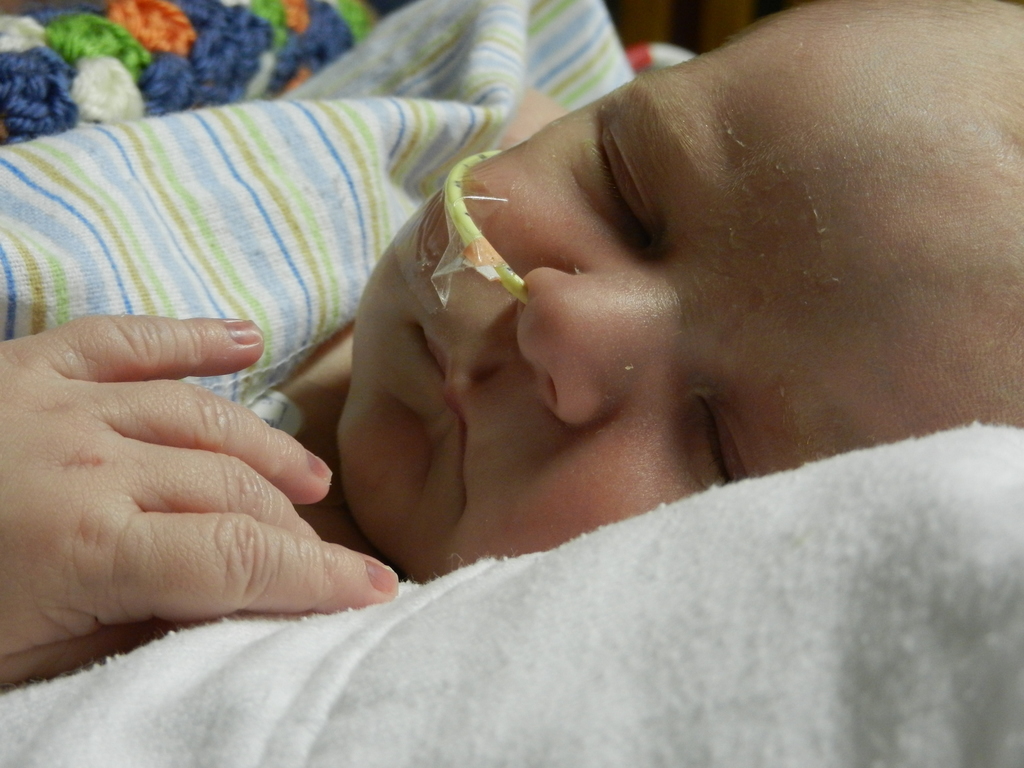
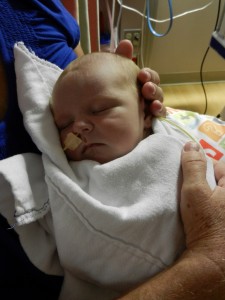
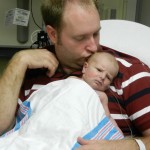
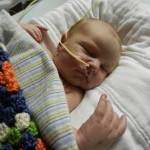
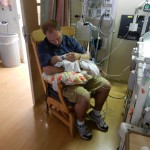
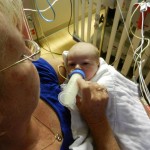
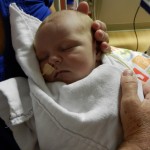
Dad had to go back to work starting Tuesday the 6th. It stinks that all of his time was used up in the hospital but we are grateful that he was able to be there and not have to use vacation, which we are both saving for the second surgery. He does have more of an opportunity to have a flexible work schedule and has been able to be around as much as he can, which is very helpful. I love being able to be home with baby boy, even if it is tiring and feels unproductive at times. Just relishing in those itty bitty baby moments makes my heart soar, so I can’t imagine how much Dad must think of coming home to snuggle with Evan. I mean, who wouldn’t want to snuggle with this cutie pie? Especially when he is zonked out in a milk coma.
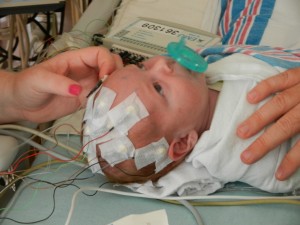
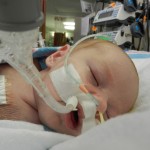
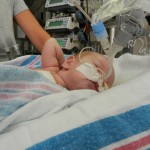
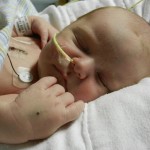
We are still working on Evan’s feeds, which apparently is the thing you do with your heart baby. We have ng tube feeding supplies but Evan has other plans and has pulled out his tube. We decided to leave it out and see how he does on his own because we truly don’t know. Doctor’s orders are to feed him 75ml (about 2.5 oz) every 3 hours, with a total of 600ml at the end of the day. He is drinking unfortified breastmilk (mine tested between 24-30 cal/oz) and is doing OK but never really hitting goal. He is closer to hitting it some days more than others. We are concerned about his weight gain, or lack of it. A visiting nurse is also coming to the house 1-2 times a week and he is weighed at this appointment along with cardiologist and pediatrician appointments so maybe because so many scales are being used it is not providing consistent and reliable data. Maybe it is becoming a bit over-analyzed at this point. At our cardiologist appointment on the 12th, we voiced our concern about feeding and weight and our doctor wants us to keep the tube out until our appointment next week and see how he does. She feels the ng tube can do more long-term harm than good and she believes that if Evan truly needs assistance in getting his caloric intake, he should be fitted with a g tube. I’m not too excited about that idea so hopefully Evan was listening and will kick up his feeding a bit.
The rest of the cardiologist appointment went just as planned. The shunt looks great but she wants to keep an eye on it so we will have weekly cardiologist appointments. The echo on his heart showed that everything still looks like it should. She looked over his meds and agreed at the amounts. His heart med, captopril, is a compound medicine and there are only 2 pharmacies we can go to to get it refilled, so I’m glad we found that out. Uneventful is good. 🙂 The next day we had the visiting nurse stop by and of course you think of more questions when you aren’t at the doctor’s office. I asked about his potassium levels because when we were in the hospital they gave him potassium pretty frequently because the diuretic furosemide that he is on can deplete it. She’s going to check with the cardiologist. I am also on the lookout for dehydration since he does not seem to have the same huge pee diapers that he was having after a dose of furosemide. Other than those very minor things, he is just wonderful.
Evan and I also tested out a moby wrap that a friend is letting us borrow. I still need lots of practice with it but so far he really likes being in it. It is a bit warmer than I had thought and the material is pretty stretchy and it is supposed to be that way but after wearing it for a bit it tends to stretch too far so I need to make it tighter. Evan doesn’t appear to mind too much tho 🙂 We also gave Evan a bath in his new big boy tub. Previously he had only gotten sponge baths so immersion in warm water was a new adventure for him. He kept looking at us with a “what the heck are you people doing” expression. No crying or fussing but plenty of big-eyed expressions. Afterward, however, he gave us the signal to get him clothed and bundled up as quickly as possible.
Pretty Cute from William Wood on Vimeo.
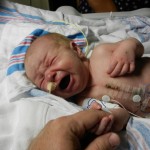
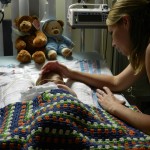
Evan was sitting with mom and was a very happy little boy, until he got hiccups.