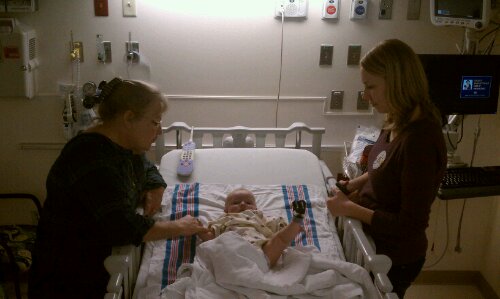
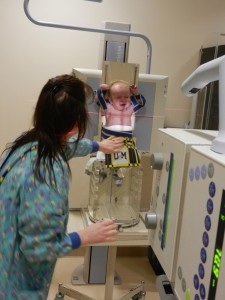
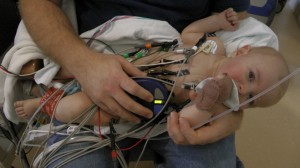
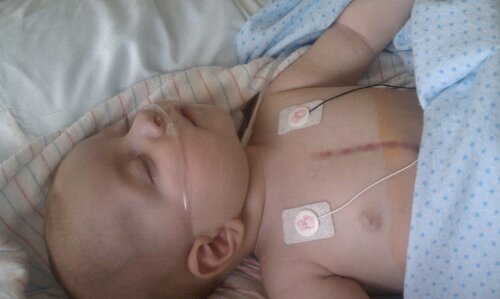
We have had a couple pretty good days. Erica was our nurse on Thursday, she was our favorite nurse from our previous stay. Evan continued to rest and recover. Erica sat him up hunched over some bundled blankets and he really loved it. He spent most of the day sleeping sitting up or sitting there looking at everything going on around him. Everyone was so enamored with our little man and how cute he was when he was sleeping but how serious he looked when he was awake. Sitting up helped some more fluids drain off of his chest and put us in great position to remove the chest tube on Friday. We found a burn and blister under Evan’s neck, this can happen if the Betadine solution they use prior to surgery for disinfecting the area is not all wiped up. We have some burn cream that we need to apply 3 times a day. I’m sure this doesn’t feel good and being under his neck there it’s never allowed to get any air because of Evan’s little neck rolls. Evan continues to be on constant pain meds, Tylenol, Motrin, Oxycodone are scheduled so that he’s never without something and the occasional small dose of morphine if he seems to be in pain.
We knew that Thursday would be our last day in the ICU, it was just a matter of when a bed would open up. We were not in any hurry to be honest. We like the 1 on 1 attention in the PCTU much better than that of the care you get on the general floor. I’m not saying the care is bad, it’s just that things don’t get attended to nearly as quickly because a nurse has 2 other kids to tend to in addition to yours. Alarms and cries go much longer before they are attended to, so I feel really guilty when I am not here. I don’t want Evan to lay crying for who knows how long before a nurse comes in to see what’s going on. Finally at about 7pm on Thursday a room opened up and we were transferred to the general floor. Oh and FYI… when I say general floor, it’s more like general cardiac floor. All of the kids around us are heart kids. All of the 11th floor is cardiac and much of the 10th is as well including the 31 bed (currently only enough staff for 17) PCTU. The picture on the right is of the television screen on the wall in our room. This TV is our portal to many movies, hospital videos, internet, and we’re even able to order food.
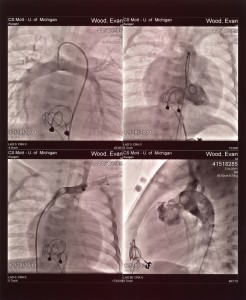
Thursday night was an interesting one… full of gas and runny stool. TMI? Evan had the worst diaper we have seen so far, it was like a lake in his pants. We had to change his bedding and a couple of his bandages because it was everywhere. All over his chest tube, g-tube, femoral IV, it was really bad. I have a picture but I’ll save you from that, LOL. Drainage from his chest tube had slowed to less than 10mL per shift so it was decided to take the chest tube out. This was done on Friday morning and Evan seems to be much happier without it. Additionally, Evan had an echocardiogram and EKG done and the results from them were normal. They did see slightly reduced function of his heart than what they saw pre-op but I would expect that since they hadn’t restarted all of his heart meds. They have since restarted his meds and his feeds have continued to go up. We’re doing continuous feeds with a pump at the recommendation of the gastroenterologists, who we’ve consulted about all of the puking that Evan as been doing.
We’ve made some friends during our stay here. Brian and Kim Sidlauskas have a son Ethan who also has a CHD and is here for another surgery. Kim and Sarah actually went to high school together. They have spent much more time at the hospital than we have, little Ethan was here for a solid 6 months the first time and Ethan had to go home with a trach and ventilator. All of that is gone now and Ethan is recovering from his next surgery and is doing pretty well. Please keep this family in your thoughts and prayers as well. We met another family while we were here as well, the daughter’s name is Avery and at their 2 month checkup the pediatrician heard a murmur, they had heard this before but didn’t give it much merit because the whole family has murmurs the pediatrician continued to look into it and it turned out that Avery had to be rushed to Ann Arbor and scheduled for immediate surgery to repair her heart. I’ll have to find out the name of her condition again, but in general, many of the arteries and veins around the heart were in the wrong place and connected to the wrong things, additionally there was an extra artery going up her neck that needed to be tied off. She had surgery Tuesday morning (this was the case that bumped us from 1st case of the day to 2nd) and is doing well. The family is now on the general floor a couple beds down from us. Mia Wilson continues to fight allusive infections, and now osteopenia which is low bone mineral density, this was found out after it was realized that poor Mia had a broken bone in her leg.
Friends from Lansing came to visit today, Tony and Jennifer Knapp. We visited with Evan for a while, went and had some dinner, and visited with Evan some more. I see that look in Jennifer’s eye, like she wants to steal my baby. 😉 We saw our first smiles since before the surgery today, thanks to Jennifer. Thanks for coming you guys, it was great seeing you.
Our hurdles before going home, in my eyes are:
- Getting him off of oxygen, so far they have attempted to wean him and each time they do his SATs drop and he needs to go back on the oxygen. We want to know what’s going on with that.
- Consult with GI… we met with them and a GI study was mentioned but I don’t think it was scheduled because Evan was on Morphine at the time. Are we going to get the study before we go? Are we going to leave and come back in a week or two once he’s settled and not full of pain meds? Or are we going to skip it since they can get copies of the studies done at Bronson? Do the Bronson ones show enough of what they need to see?
- We need to know what to do with his feedings. GI said that we should continue doing continuous feeds on the pump for a few days and then start progressing towards bolus feeds (bolus means all at once) but we don’t have a scheduled or know exactly how to do that. Nor do we have a feeding pump or know how to use one.
These things could be figured out pretty quick so we could go home yet this weekend or on Monday.. Less than 1 week in the hospital?! Evan, you are amazing.
Here are some pictures from the last couple days.