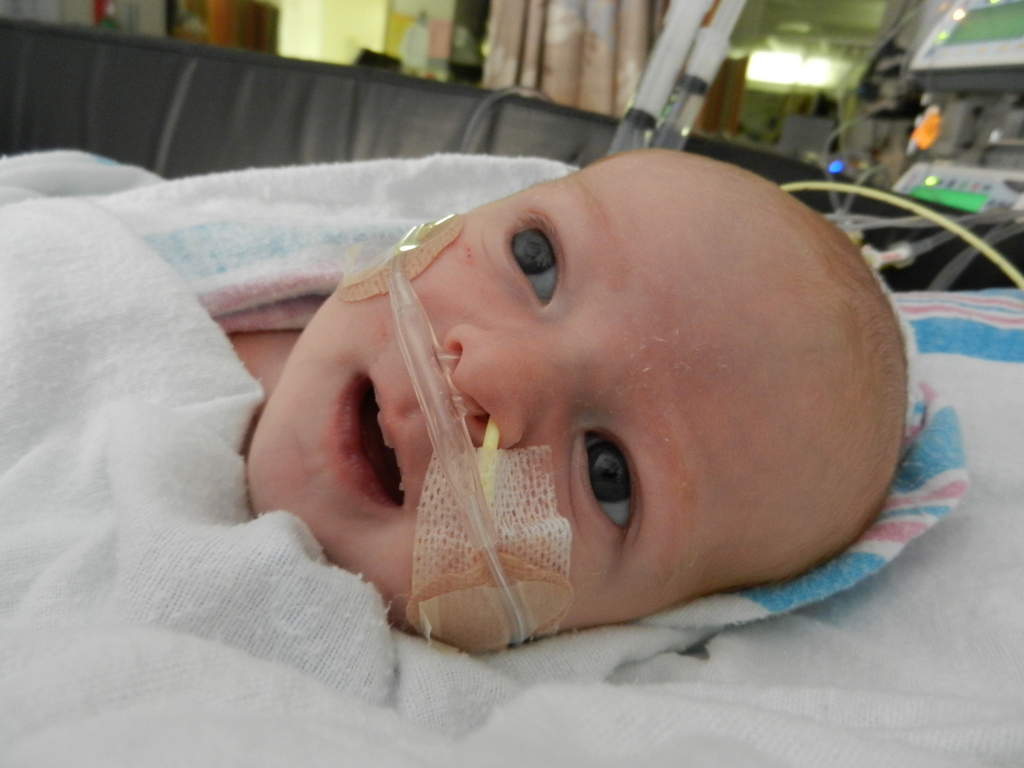
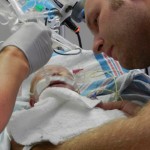
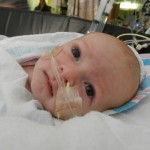
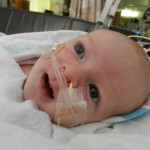
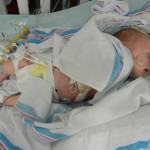
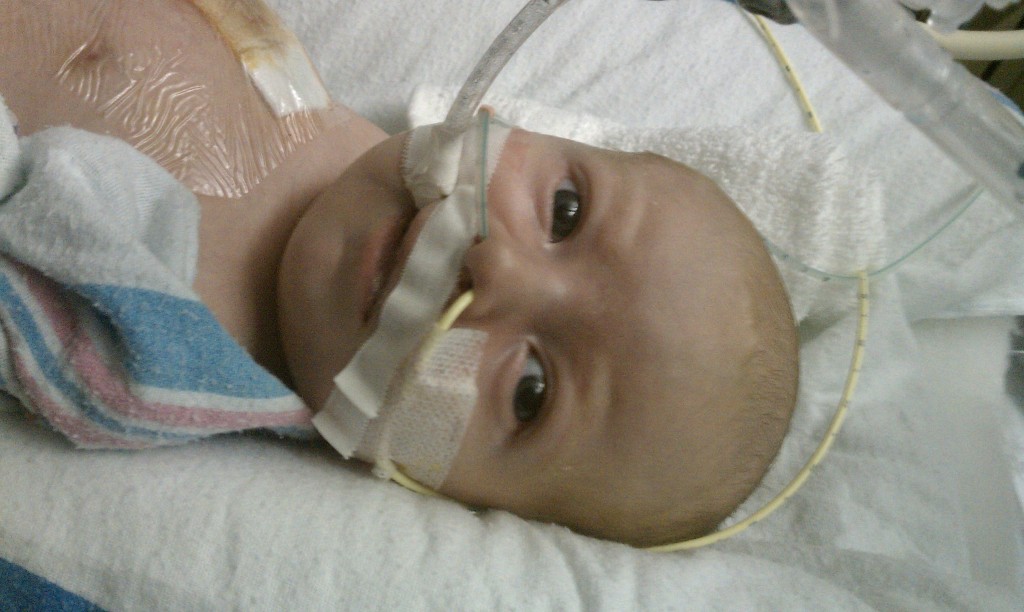
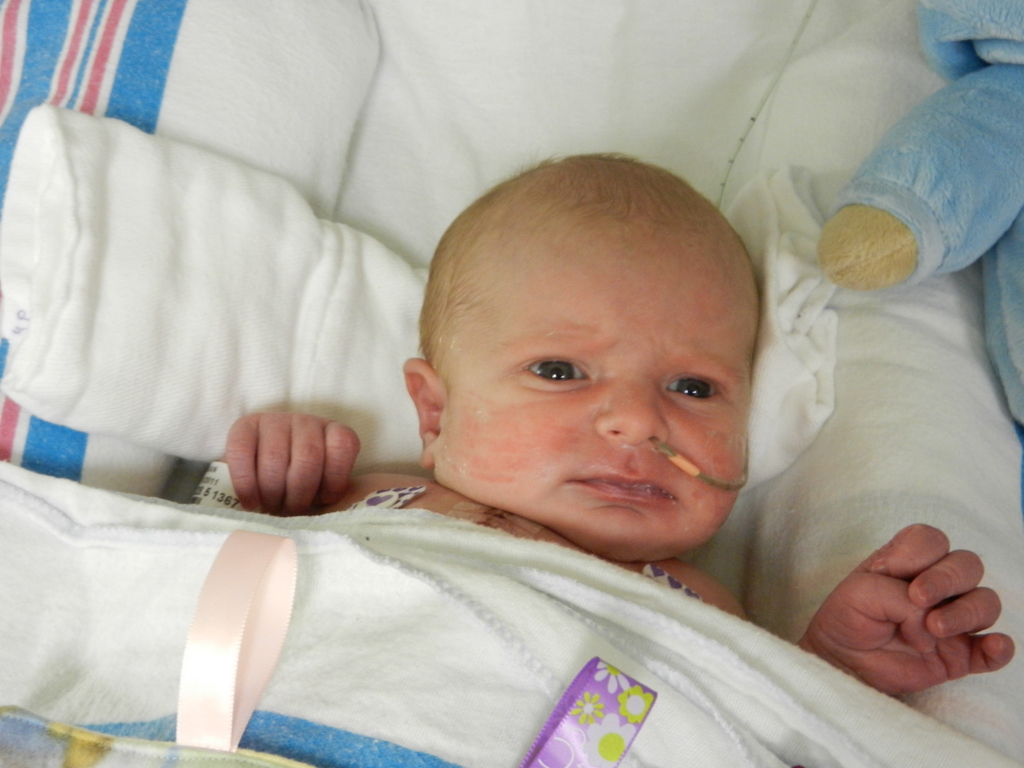
Being in general care is pretty nice. The room is a typical hospital set-up; 2 beds in the room separated by a curtain running down the middle. There is also a couch that can be used for a bed, meaning Evan would be able to have an overnight visitor. I elected to stay overnight with him and give this whole sleepless Mommy thing a trial run. We had a midnight feeding and then got all settled down and sleeping around 1ish. Evan had another feeding at 3am and the nurse must have just set it up to be a tube feeding because he was sleeping. I woke up to Evan getting restless and fussy in the middle of this feeding. That isn’t all too uncommon for him. He has his own personal internal limit and then anything beyond that makes him fuss for a little while and then he calms back down and usually sleeps through the rest of the feeding. He did that and we eventually got all snuggly and sleepy around 415am.
Wouldn’t you know but of course at that time the sticky electrodes on his chest for his ECG decided to randomly not be sticky anymore and his alarm kept going off. Now, the thing about general care is that the nurses have a lot more patients to take care of so the response isn’t the most immediate. It was going off intermittently for about 10 minutes and then it was silenced once and for all. I cannot wait until we aren’t hooked up to things anymore that give false positive results and make a whole lot of noise for nothing.
Evan is still battling a cough as a result from coming off the vent. He sounds junky, like he would have a bad chest cold. About 10 minutes after settling him down from the alarm he had a series of strong coughs. It’s great that he is working on getting things out of his system but they must still hurt a bit to cough that hard, so he was awake and upset. He calmed down easily again at around 5.
At 520ish, a nurse came in to draw some blood. Now, because he still has lines she did not need to poke him or anything but the lines were firmly underneath the blankets and he was fast asleep. No more… the nurse woke him for the blood draw. He was very restless, more than usual and it took quite a while to get him calmed down. There was nothing apparent that was wrong. We slept off and on with continued interruptions from the nurses and as the early morning wore on he became more and more irritable and more and more difficult to console.
Will got to the hospital at around 9AM and took over with him so I could get some sleep on the fold out couch next to the bed. Here is his account of the rest of the day up until now:
Evan did not want any part of his 9AM feeding that Sarah had been trying to give him in a bottle since about 8:30AM when he woke up crying so I setup the feeding tube and took over rocking chair duties from Sarah. He was extremely fussy, much more than normal. No matter what I did he was not calming down which is pretty unusual for him, he’s normally so easily consoled. The small grunts on every breath turned into full blown screaming and crying that lasted for quite some time. The nurse practitioner was called in as well as the current attending doctor on the floor who just also happens to be one of the electrophysiologist’s, Dr. Martin LaPage. They wanted a quick chest x-ray to check for fluids around his heart and an echo to look at his heart function. While they were waiting for people to show up they ran a blood gas and that’s when all hell broke loose, there must have been 8 people standing around his bed. His lactate was at 20 (should be 0.6-1.5) and his pH was down to 7.0 down from 7.40. This was pretty alarming to the doctors and they busted ass back to the ICU. Evan was put back on the ventilator and all the lines that he just got out were put back in so they would have access for medications. They stabilized him pretty quickly with medications and he’s comfortable. They have ordered/performed/planned several tests. They took saliva and urine samples for more cultures. Three x-rays. And as I type they are doing a very extensive fetal echocardiogram. Three people have been at the helm of the echo for the last 45 minutes or so looking at everything. Doctors from pediatric surgery came down and examined him as well. Given the problems that he’s had with feedings and and the susceptibility of these kids they are thinking that it might be Necrotizing enterocolitis(NEC). This is not good… this has been a huge fear of ours. The little girl that I mentioned in my previous post, Eva, she has several bouts of this. We’re not coming home this week and if it turns out to be something as serious as NEC then we won’t be home for quite some time. I’m being kicked out of the ICU because they are bringing another patient back, so I am going to stop it here… i’ll keep posting as we hear more. Keep the sweet little boy in your thoughts and prayers.