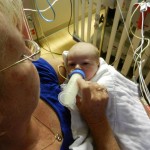
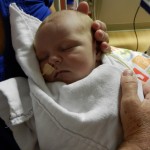
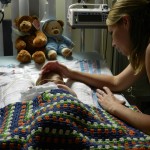
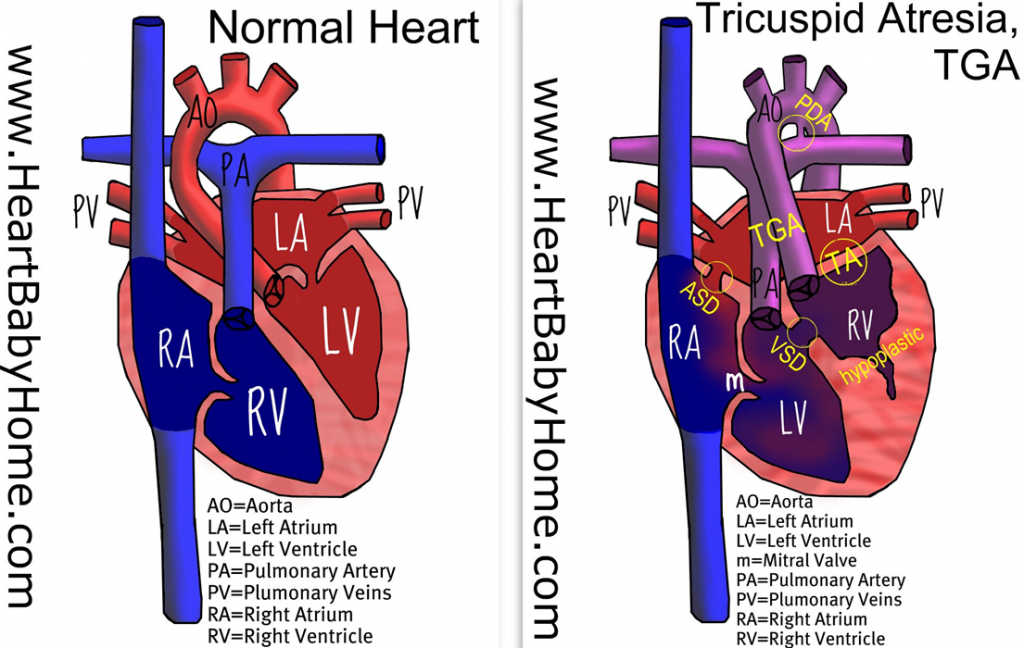
The short of it: Evan had a seizure early this morning and several more throughout the day. They are the result of a stroke he had some time ago but not sure when. He is comfortable, sleeping, and stable. His brain activity is being monitored continuously for 24-48 hours. He is NPO again (removed from feeding). We were scared but it appears he is ok for now. Here is how we got here…
I received a phone call at 4:45 am from a cardiology fellow. Overnight calls while your child is in the hospital are never a good thing. I was so out of it that I didn’t answer the phone, but had my bearings enough to immediately listen to the voicemail he left. Heart racing, I learned that Evan had a seizure and that he was currently undergoing a CT scan. Thank God he said the phone number for Moderate Care twice so I could make sure the reality of what I was doing was not some scary dream.
I called Moderate Care and spoke to nurse practitioner Denise who gave further details on the fellow’s message. She explained that at around 3 this morning, Evan’s oxygen saturation alarm was going off. The nurse suspected that perhaps the pulse ox band just came undone (it does happen a lot, but mostly when they are awake and moving or when you are holding them and moving around.) When she came to check it out, she noticed that Evan looked “mottled and dusky.” She took a blood gas sample and gave him oxygen. His pH was a little low, lactate was ok. After a little while he started doing better and became more responsive. The plan was to take another blood gas in an hour and see how it looks at that time.
At 3:30, the nurse went to reposition him and have him sit in his Boppy. Suddenly he stopped crying and moving, his breathing became sleep apnea like, his head moved to the left, his eyes deviated off to the side. She said he went “unresponsive” and called the cardiac fellow in to look. They pulled another blood gas and this had a better pH, lactate was still ok, white blood count was normal (indicating no infection), hematocrit was fine (indicating good response to transfusion yesterday), and his potassium was a little low so they gave him some extra. There was a concern he was having a seizure so they started him on phenobarbital. His feeds were turned off and they ordered a CT scan (he can’t get a MRI due to his pacemaker, but I think the CT is the default test).
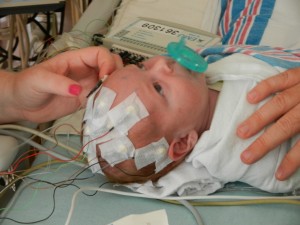
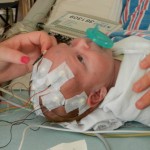
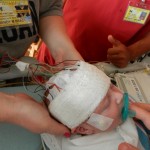
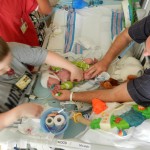
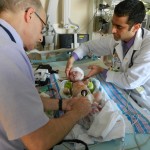
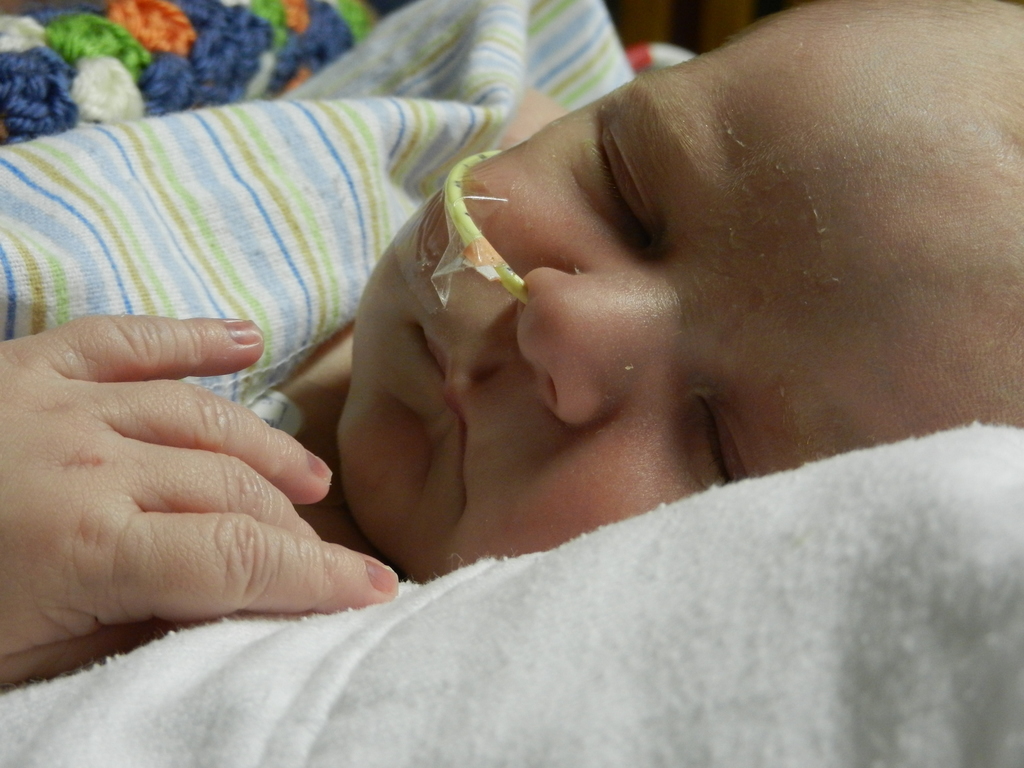
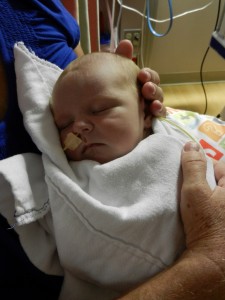
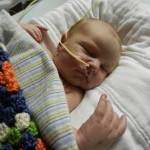
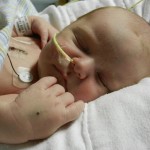
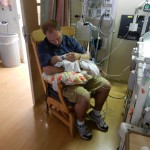
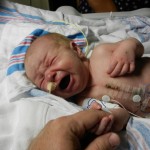
By the time we got to the hospital at 6:45, Evan was already back from his testing, his birthday balloons detached and bunched together because they had to move him in his bed for the procedure. He looked completely normal, still had his feeding tube in (which Evan ripped out but that’s for the better considering he is NPO again). I got to snuggle with him until 8:30 (Dad is feeling sickish and wants to keep some distance) until I had to step out for a bit. When I came back at 9 people had arrived to place Evan on EEG or Electroencephalogram. They are going to continuously monitor his brain activity for 24-48 hours, depending on what they see. Additionally, he is being video and voice recorded as well, so they can see what happens when he has one of these fits.

At 10:30, Dr. LaPage, the electrophysiologist, came by to check Evan’s pacemaker setting. He has been having low diastolic blood pressures today and they wanted to see if raising his heartrate from 110 to 120 would improve this value. It didn’t so they left it at 110. When your heart is in diastole, it is filling with blood before it contracts again. Your diastolic BP is the lower number. The fear is that a low diastolic BP may have contributed to his previous cardiac episode on the 16th, so they’ve been monitoring this value as well. It had normally been in the 40s but it was in the low 20s when they started trying to make adjustments. Its a teeter-totter balance between pacemaker rates and medications.
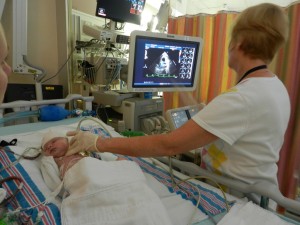
An echo was ordered to see if perhaps there is something lingering with his broviac, a catheter placed into his heart during his first surgery. Perhaps a blood clot formed and traveled to his brain – the nurse suggested. Wait – blood clot? That sounds like a stroke. Thought we were talking about seizure here. A thorough echo was performed around 1:45 pm. It was perhaps the clearest images of his heart we had ever seen and we were pestering the technician with structural questions. “We’re nerdy science people who didn’t go into medicine,” is our explanation.
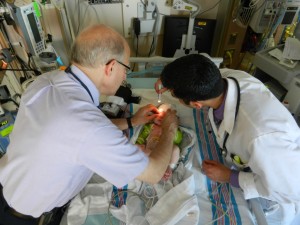
During the echo, the neurologist, Dr. Leber, and a fellow came to talk to us. During the conversation we talked about the CT scan images and he said, “Do you want to see them?” Why yes, yes we do. The majority of the questions resulted from the images. Evan had a stroke, not yesterday and not when he was born, but sometime. The doctor did make a comment like it might have happened “a week ago.” Hmm a week ago… what happened then… Oh that’s right his cardiac incident where he went critical with acidosis and was rushed back to PCTU. Unfortunately this is the only CT scan we have so we can’t compare to anything, but Evan did have an ultrasound performed on his head the day of his surgery and when looking at those images (although not nearly as easy to see) the doctor did not see any damage at that time. Damage. Yes, Evan has some on the left side of his brain. On the CT images, it looks quite large.
 This isn’t Evan’s brain and I think it is a “normal” adult one but I’m not sure. I just drew this up for visual reference. A CT scan is like slices of your body from your toes to your head, so when you look at images of the brain its like looking up someone’s nose. The left and rights are backwards. The area of injury permeates through several “slices” of Evan’s brain. The image I drew would be the damage at its largest. As you travel the slices toward the top of his head or toward his toes, the area tapers in dimension. CT scans are gray in color, and the damaged areas turn darker gray. White is the skull. Black is water and having some at his age is ok.
This isn’t Evan’s brain and I think it is a “normal” adult one but I’m not sure. I just drew this up for visual reference. A CT scan is like slices of your body from your toes to your head, so when you look at images of the brain its like looking up someone’s nose. The left and rights are backwards. The area of injury permeates through several “slices” of Evan’s brain. The image I drew would be the damage at its largest. As you travel the slices toward the top of his head or toward his toes, the area tapers in dimension. CT scans are gray in color, and the damaged areas turn darker gray. White is the skull. Black is water and having some at his age is ok.
So what will the damage be? It is hard to say in a baby this young. If it were you or I, the doctor said we might have trouble feeling our right leg, hand, or right side of our face. We might have trouble with verbal comprehension but not talking. We might have issues with being able to name/identify our fingers on our hand. We could have attention problems. Who knows how this will affect Evan. His brain is growing so rapidly that maybe no damage will be done. We don’t even know his handedness yet (I’m thinking southpaw but that’s just me). There is another area of concern on Evan’s right side as well. Evidently, as the damaged stroke area gets older, it gets darker in the CT scans. There is a slightly shaded area on his right side that would be indicative of a separate stroke incident if it turns out to be something. They are going to check in a week to see if the area darkens and to confirm if there was another stroke (think of the stroke areas as slowing developing polaroid images). Even when he is 20 a CT scan will show a dark area on his left side from the confirmed stroke region. It might get smaller, but it should get darker. The neurologist said that in adults the area retains a brain look but in babies it often disintegrates into a watery slush (?) but couldn’t say why this is so. Water on the CT scan looks black, so as he ages it should turn into a blackened mass.
The treatment for now is to continue to monitor the seizures on the EEG. Seizures can damage the brain cells on the fringes of the stroke region. Or it can further damage blood supply to the stroke areas thereby causing more damage to previously unaffected areas. If they see more seizure activity, they will manage that with phenobarbital doses. We asked about other medications but that is the best option for babies. In looking up seizure medication lists there are a lot of familiar names. Phenytoin Sodium anyone? More of the wait and see game.
And just after the conclusion of all of this, a nurse drops a package off at Evan’s bedside table. A gift from the VanEseltine family. Lots of tears. Many thanks. Your support, thoughtfulness, and kindness means everything to us and it couldn’t have come at a better time.
Results of the echo are fine. There are no indications of a clot on his broviac or associated with the heart. Maybe there was one and it was missed before and that traveled to his brain? The neurologist said it is possible that happened before, but this latest echo again did not show any smoking gun. Good news is because we identified it as a brain issue, there is no need to keep him NPO so they will start feeding him sooner than later, starting over on the complex feeding protocol.
Please pray for the doctors to have the wisdom to figure all of this out. If he had 2 separate events then what is the source? Are there still more potential clots out there? Could there be more events? How much longer will the seizures last?