You know it’s time for an update when you wake up to several messages on Facebook, text messages, and a voice mail…Sorry I have been slacking on the updates.
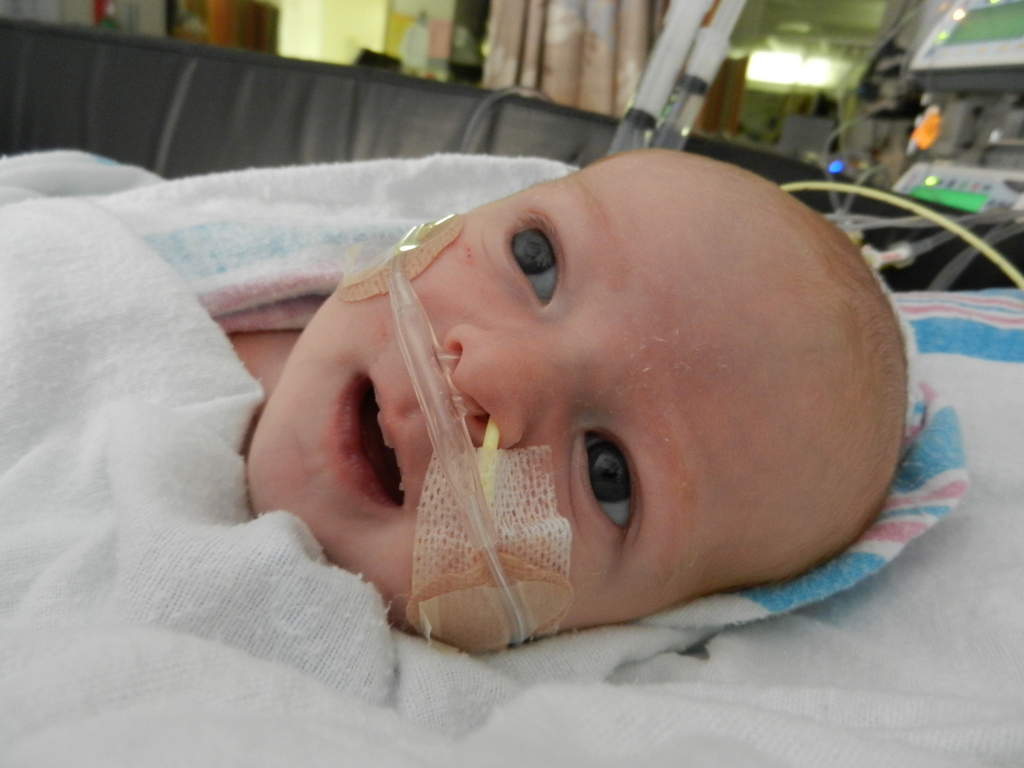
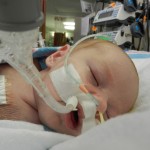
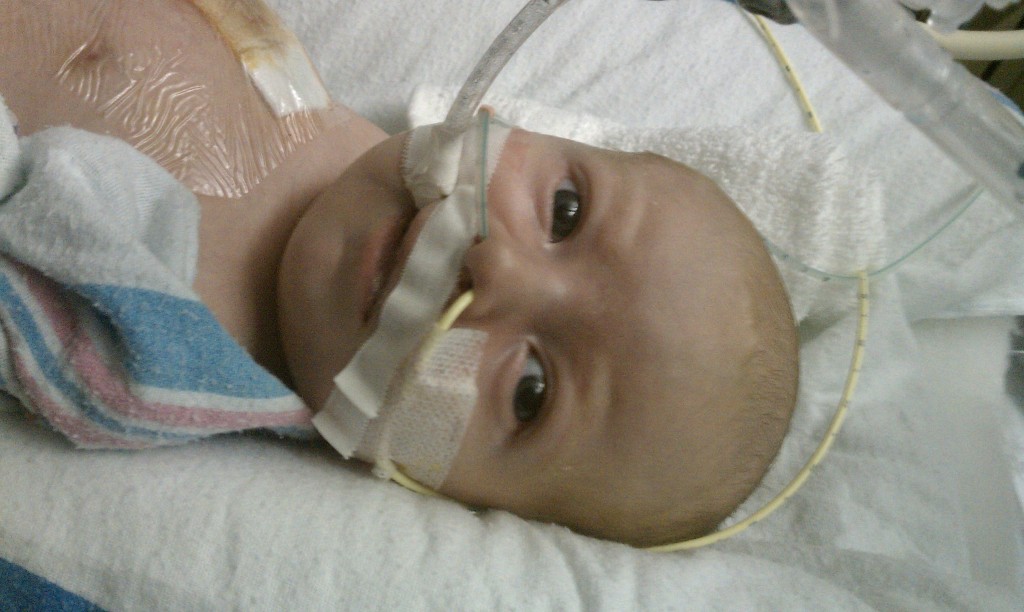
 The truth is there has not been much going on to tell you other than he’s cute and cuddly, but you already knew that. The plan last week was to wait until Monday (yesterday) and make the decision on whether or not Evan needed a pacemaker. Well, wouldn’t you know it, Monday morning his own rhythm starting overriding the external pacemaker. The pacemaker is set to 100 bpm (beats per minute) and his little heart was going at 110-125 on its own! (Normal newborn heart rate is 120-160) Unfortunately it was short lived and was still not a regular rhythm. It did give the doctor’s hope that maybe he’s no longer in complete heart block and it’s only partial. They want to give it a couple more days and see what happens. <sigh> It should be a good thing, but we’re not very hopeful that it’s going to change enough to make a pacemaker unnecessary. At this point it seems like a pacemaker is the best thing for him and would make Sarah and I feel much more comfortable taking him home. Since yesterday morning I have not seen him override the pacemaker and when it was turned down his underlying rate was in the mid 70’s again.
The truth is there has not been much going on to tell you other than he’s cute and cuddly, but you already knew that. The plan last week was to wait until Monday (yesterday) and make the decision on whether or not Evan needed a pacemaker. Well, wouldn’t you know it, Monday morning his own rhythm starting overriding the external pacemaker. The pacemaker is set to 100 bpm (beats per minute) and his little heart was going at 110-125 on its own! (Normal newborn heart rate is 120-160) Unfortunately it was short lived and was still not a regular rhythm. It did give the doctor’s hope that maybe he’s no longer in complete heart block and it’s only partial. They want to give it a couple more days and see what happens. <sigh> It should be a good thing, but we’re not very hopeful that it’s going to change enough to make a pacemaker unnecessary. At this point it seems like a pacemaker is the best thing for him and would make Sarah and I feel much more comfortable taking him home. Since yesterday morning I have not seen him override the pacemaker and when it was turned down his underlying rate was in the mid 70’s again.
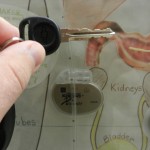
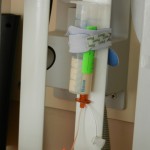
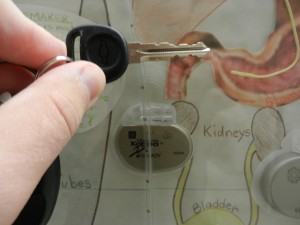
The picture on the left is from a display case outside our room that shows all kinds of medical devices that are common in cardiac kids. This particular shot is of a pacemaker. You can see how small it is in comparison to my car key.
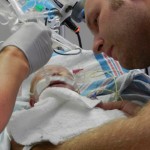
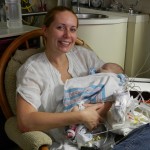
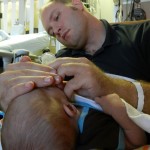
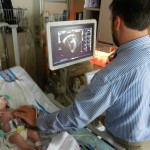
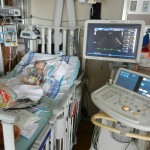
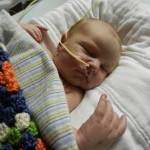
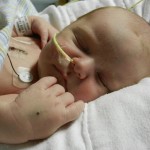
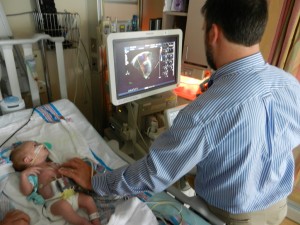 Evan had his first echocardiogram since the surgery. He was not a happy camper, although he was not very happy in general yesterday. He calmed down after about 5 minutes and let the man do his job in peace. We heard some results this morning which were good. The shunt that was placed looks good, no issues there. There is some very minor leaking in a couple of his valves which is not a concern, just something to watch.
Evan had his first echocardiogram since the surgery. He was not a happy camper, although he was not very happy in general yesterday. He calmed down after about 5 minutes and let the man do his job in peace. We heard some results this morning which were good. The shunt that was placed looks good, no issues there. There is some very minor leaking in a couple of his valves which is not a concern, just something to watch.
I was sitting in a rocking chair with Evan and after I got up and put him in the crib that my stomach felt cold…and wet. Diapers leak, even the good ones, end of story.
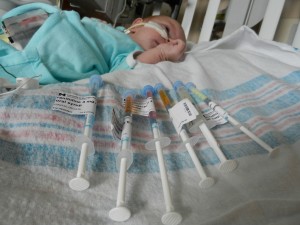 Evan has been promoted to all oral medications, but he still has several. A couple diuretics, aspirin to prevent clots, Reglan to promote digestion, Tylenol and/or Motrin for pain, and Zantac for acid reflux.
Evan has been promoted to all oral medications, but he still has several. A couple diuretics, aspirin to prevent clots, Reglan to promote digestion, Tylenol and/or Motrin for pain, and Zantac for acid reflux.
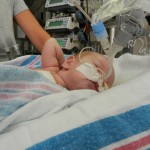
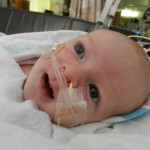
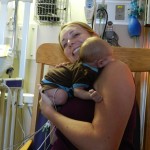
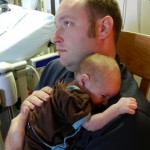
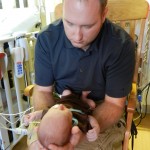
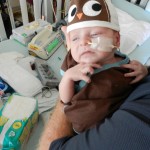
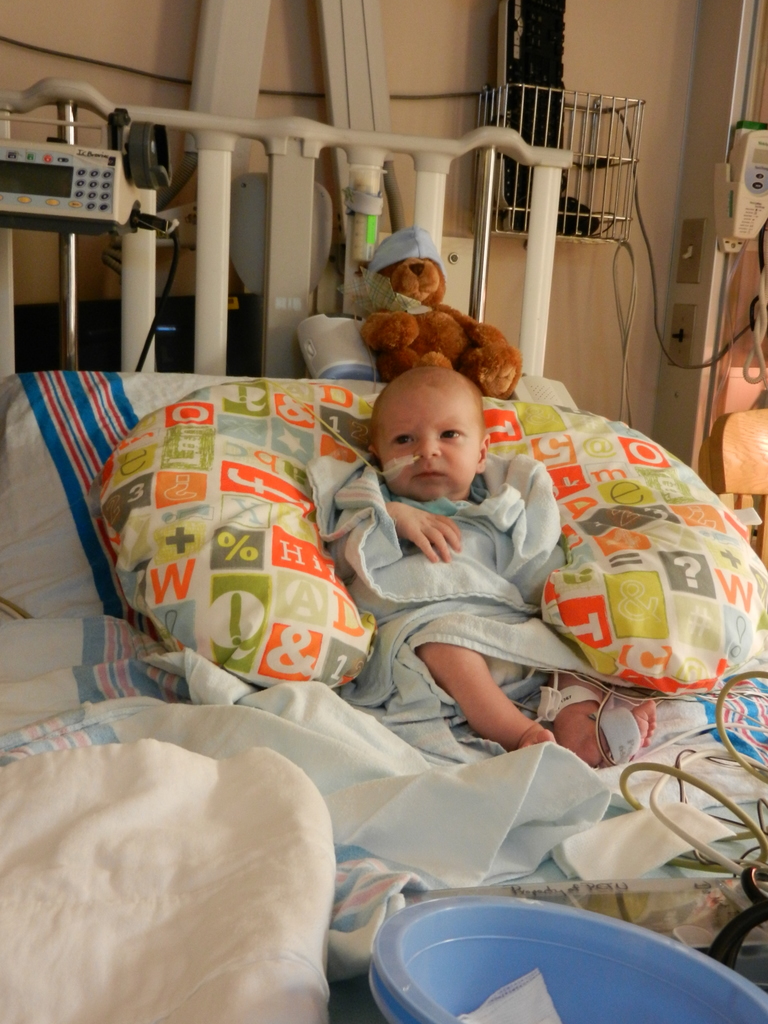
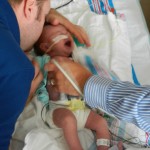
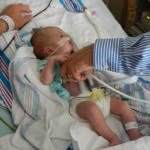
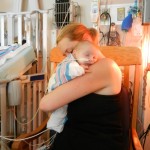
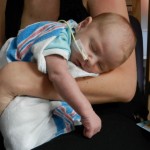
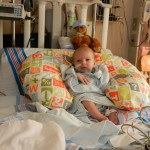
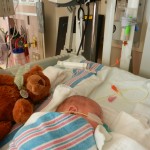
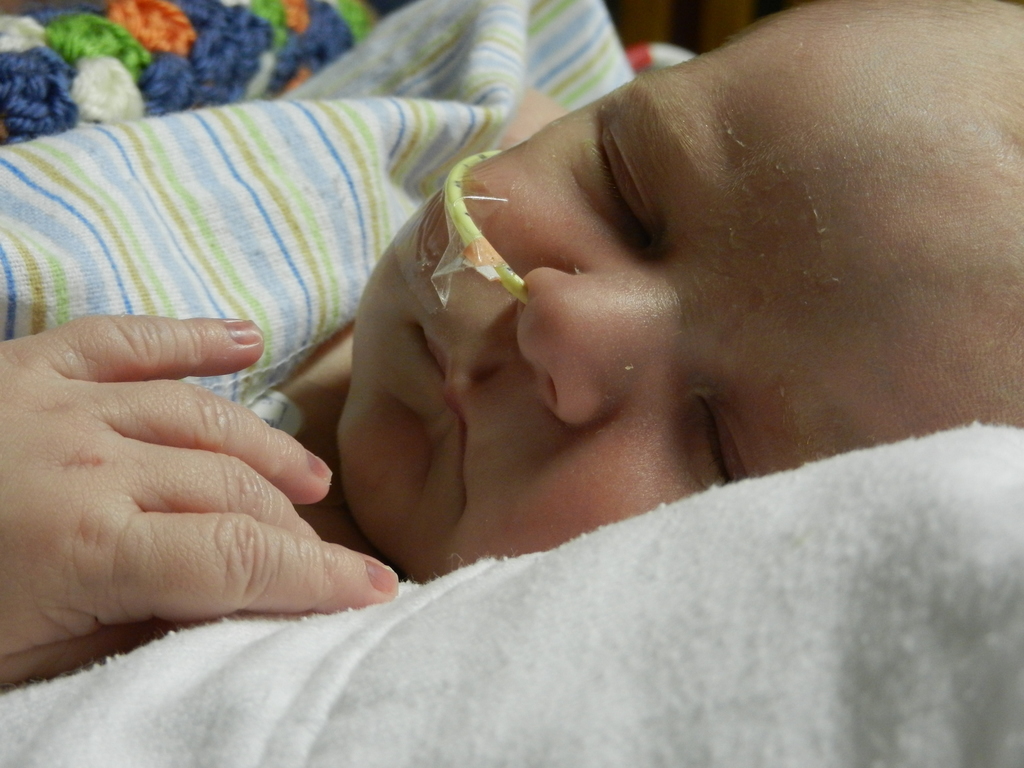
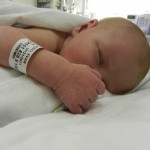
Evan loves to look around and loves to sit up. He can hold his head up a little bit and moves it from side to side to look at things. We sat him up in the Boppy and he looks around the room in amazement at everything he sees. Yesterday he watched some Family Guy and some Bachelor, nothing but quality television for our son.
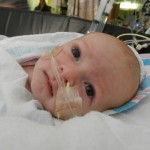
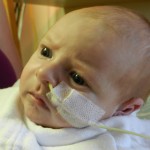
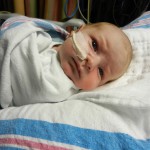
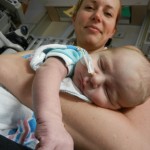
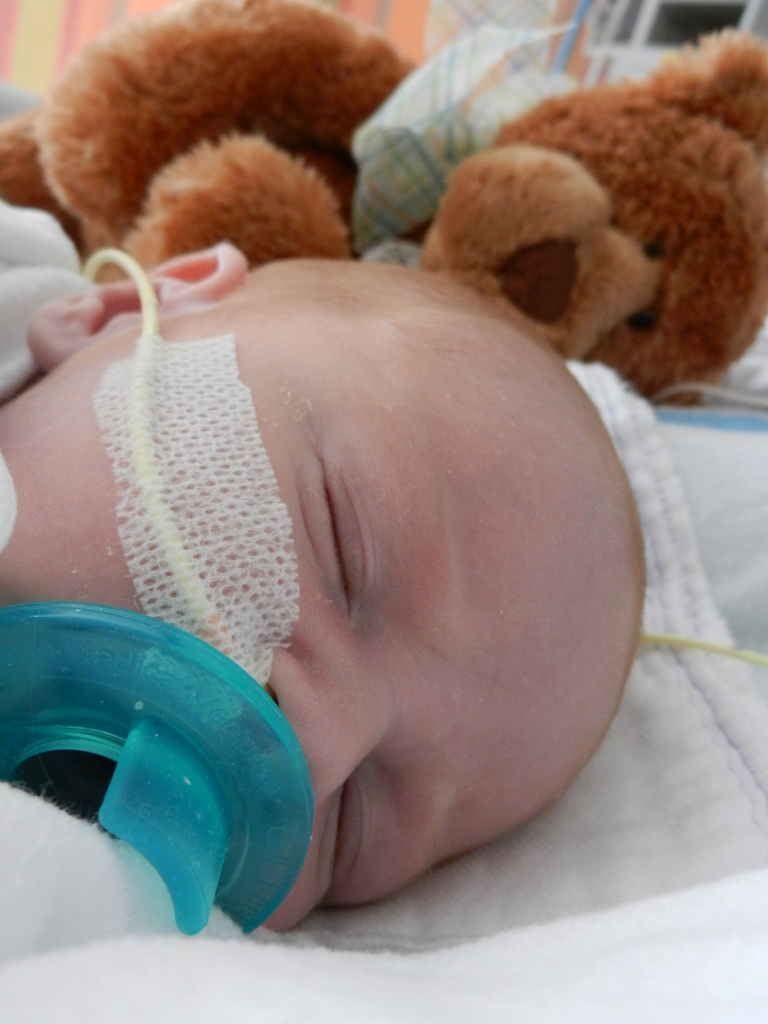
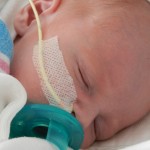
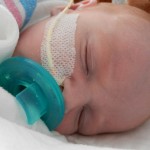
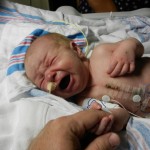
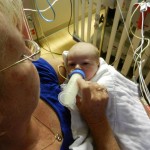
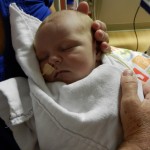
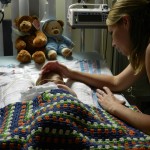
Click on any of the images below to see them larger. (is that red hair that I see? are we going to have a little ginger baby!!? ohhh no, it’s strawberry blonde, it’s strawberry blonde…)
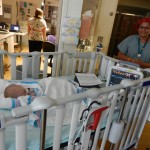
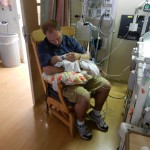
 It may not seem like much, being one month old… but given what Evan has gone through in his short time here we wanted to celebrate a little.
It may not seem like much, being one month old… but given what Evan has gone through in his short time here we wanted to celebrate a little.