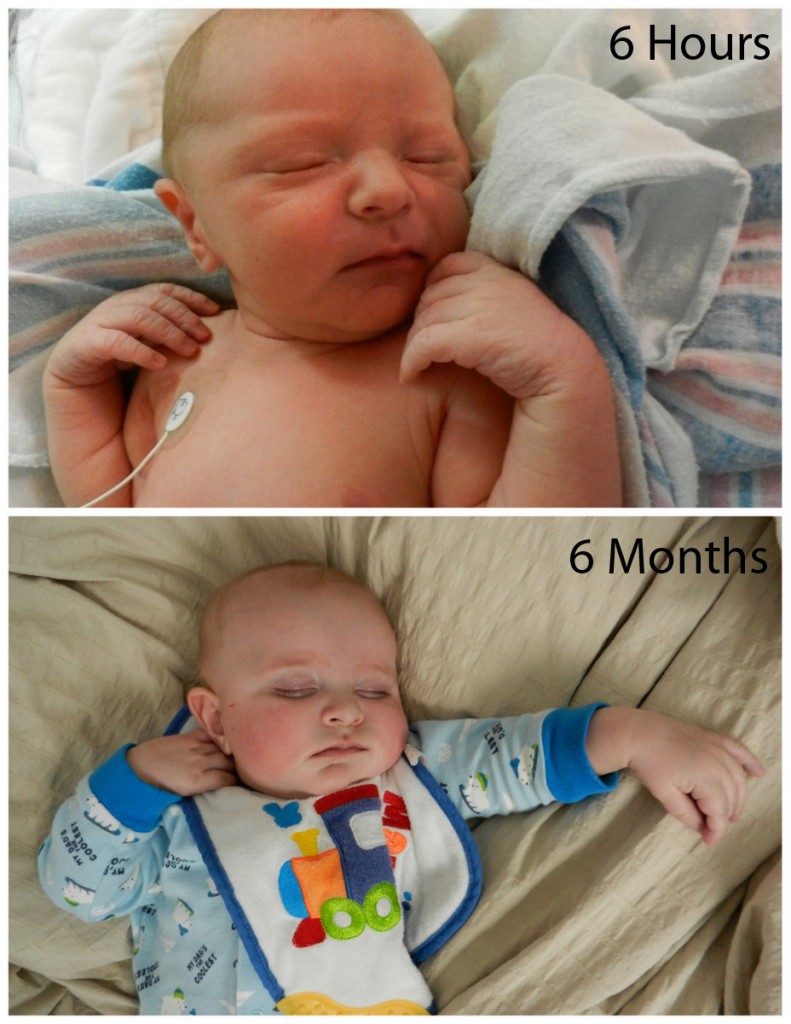
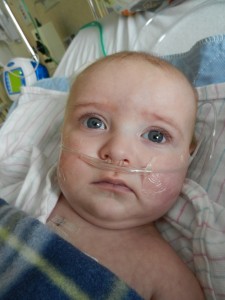
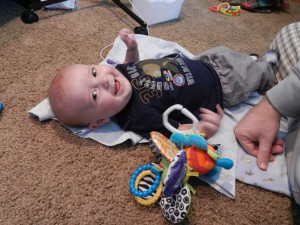
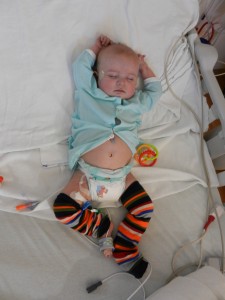
We have been home for a couple of days and realized that we have left some (non- Facebook) people in the dark. Sorry about that.
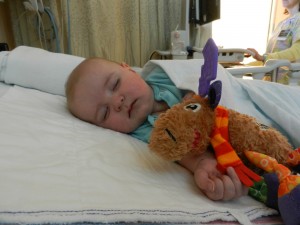
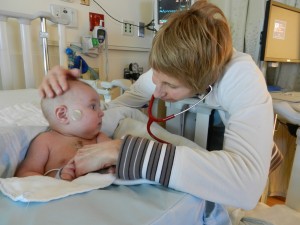
On Sunday they had finished monitoring Evan’s chest tube drainage. He received the all-clear to take it out and Will and I got to be in the room when they did it. Because he didn’t have the tube anymore, he didn’t need to be in the ICU and moved onto the floor. He also didn’t need his scheduled dose of oral morphine anymore, which was really nice because I think it was a big influence on the sluggish and sad baby we were witnessing. We had to give it 2 days and then recheck to see if any more fluid accumulated.
We were debating on whether or not to go to work on Monday. Will’s schedule was horrid for the beginning of the week and I am already in a mini-panic about using so much vacation and we aren’t even out of January yet. We were both getting ready to leave for the night when a couple of things said by the nurse just made Will and I look at each other sideways and I said, “Well I guess I’m staying here tonight.” Thank God my company and more importantly my boss is a kind and reasonable person.
The nurse had come in to change his feeding bag which was fine. She asked us if she could pour 8 hrs worth of formula into his bag instead of just 4. Hmmm. No, we said. We like to check for air because he is a pretty gassy kid (which contributes to the pukes and should be noted with his food issues). What she said may have been innocent but what we translated it was – I don’t want to have to get up and check on your kid so I’m going to pour enough food in here so he stays quiet all night. He’s was also going through a terrible terrible diaper rash (even wound care came up to check it out) so he will need to be changed when he wakes up and you can’t let him sit in it all night. Oh let me add that he was having crazy poops every ½ hour that I’m sure was a result of the feed change and his poor butt was just so raw. So that was strike #2. And then she gets his feed bag all ready, hooks it up, and leaves. She forgot to prime his line, so all of the air stuck in the line would have been pumped into his stomach, causing further gas and puke issues. Dude! Seriously?
Listen, I understand that Evan is #1 to us, is our only child and therefore can be our only overly-protected priority. This was just unacceptable considering how tender he was at the time. He is so gaggy and pukey and we just didn’t get a good vibe at all.
Monday was whatever – another waiting day in the hospital. Something I found irritating was that Evan was still having issues keeping his O2 levels above 70 like the cardiologist wanted so they had him on a little oxygen again but they weren’t monitoring his saturations all the time – just when they got vitals every 4 hours. Is that normal? I thought it was odd that you would have a patient receiving oxygen but not monitor it all the time and rely on a few checks to determine if the level received was adequate or not. It was not a secret that he still dips into the mid-60s for a good 30 minutes at a time, even when sleeping. I’m sure they know better than me. I hope…
We were also noticing a bloody/mucus discharge coming from baby boy. Gross. We actually weren’t sure if it was some skin and tissue coming from the diaper rash sores but consistently we weren’t seeing anything come off while wiping. Then as I was explaining this to the nurse I changed his diaper and a big blood/mucus plug (I know) came from his butt. So whatever this was it seemed to be mucosal lining or something. They passed it along to the lab to have it checked for C. dif
I wanted either one of us to be there the day he was discharged and we weren’t sure that was going to be Tuesday but I decided to just take that whole day off too and be at the hospital. I don’t care what anyone says – discharge days are the most stressful days. Drs, nurses, specialists, technicians are CON.STANT.LY coming into the room, asking a billion questions, telling you important details as you are trying to get things together, take care of baby, and run over your own mental checklist to make sure they don’t miss anything (which they did – yay!) I just hate how busy busy busy those days are. Certainly don’t make it easy. Evy got his chest xray and some thought it looked the same as it was a couple days ago but to others thought they saw fluid so we had to have an ultrasound as well to confirm that there was just a small amount of fluid but no big deal. We got the all clear to leave but we had to wait for the discharge stuff to be set up.
Since we are on a special formula we needed to order that through HomeMed too so the hospital sent us home with a few cans. We also needed to go home on oxygen so they set it up with Airway gas to give us a travel bag with a tank plus have large tanks delivered at home. I mentioned the inability to measure his O2 at home because we do not have a pulse ox but I was told again that it wouldn’t be necessary. Huh? You want us to administer oxygen when we think he needs it but you aren’t going to give us a way to measure it (and yes he can get too much oxygen too)? Well someone re-thought that because they ended up giving us one (HA! suckers…) and it actually works really well. They went back and forth about having Evan on O2 all the time or just as needed and we decided all the time because putting the cannula on and off would just be torturous to him. As least we can stick it on and have it be good for a little while. He hasn’t seemed to mind wearing it at home too much.
Tuesday night Evan was super cranky and we were monitoring him and he was mostly in the 60s so we decided to put him on oxygen. It took a while for his number to stay more in the 70s than 60s but we got there. We still weren’t sure if we were supposed to up his amount or anything so we sent a note to his Cardio to hear what she had to say. I stayed home on Wednesday too so I could keep a check on his O2 and take him to his pediatrician appointment. It was supposed to be his 6-month well baby but it was mostly just to catch them up (this was the same office tho not the same doc that saw Evan the Saturday before he was admitted and didn’t hear the fluid filling his lungs despite us telling the doc several times about his left plural effusion. I want to give them benefit of the doubt and say it must not have been enough to hear but I believe he was also doing his grunt breathing at that time too… we were admitted 5 days later)
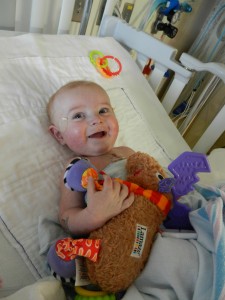
Evy was very happy all day but must be getting to an age where it is hard to leave his sight because I couldn’t leave the room without him freaking out. He still does have barfing sessions although not as numerous but they can last 30-50 minutes. His food is a liquid but somehow in his stomach it manifests into a solid so when he does puke it looks like a can of dogfood. So I get down to my last can of formula (which lasts ~5 hrs of constant feeding) and I still didn’t get my HomeMed package with more food. I call them up and ask where my stuff is at and they tell me that it will be here at 9am on Thursday. I tell the lady that as of 9pm on Wednesday Evan will be out of food and that this is special formula so I can’t just give him anything. She tells me that they don’t keep it in stock and that they had to order it to their facility (they are in Ann Arbor). She does some research and finds that there are 2 cases of this formula that they happen to have laying around that got returned from some other baby’s order. So they drove the formula and our other supplies out that night and we had it before Evan ran out. At Bronson we had a discharge lady who set all of this shit up so I don’t know what was missed. I don’t know if HomeMed didn’t realize that they don’t stock the formula and it would be another day delay on their part and didn’t tell this to Bronson. Or maybe the discharge lady didn’t tell the nurse who was handing me cans to make sure I had 2 days worth instead of 1. I don’t know but that shit is f-ed up. HomeMed has their act together so I am willing to strike this against Bronson yet again. It’s like really… I have to fight with you too??? I don’t have enough stuff to manage already???