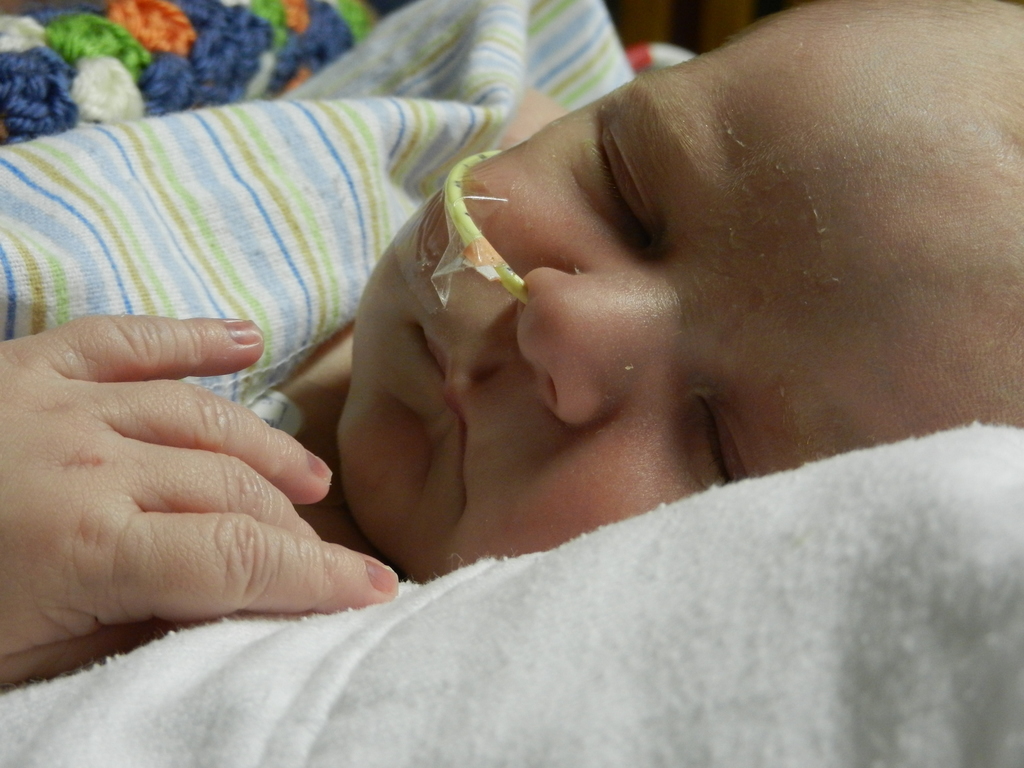
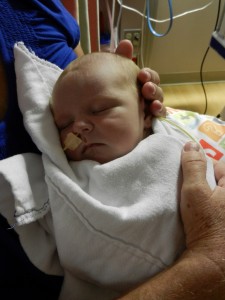
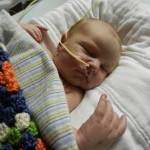
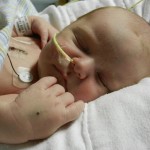
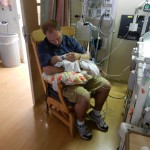
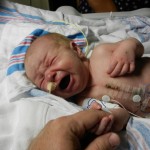
This morning Evan had a chest x-ray and everything looks great. He still has a wet-sounding cough occasionally but it must be residual congestion and is not indicative of any illness. Good news.
Evan also had another EKG and visit from his electrophysiologist. They had originally turned his pacemaker down to 80, but Evan was slightly below that so they turned it down to 70. Since then he has been pacing on his own. The docs want to collect 24 hours of his own pacing and they will evaluate the data on Thursday and make a final decision about the pacemaker.
It was put to us that Evan is in a gray area when it comes to the pacemaker. With his anatomy, he will need one. And with a low heartrate, he will need one. The question is when. He appears to be tolerating the low rate well. He does sleep a lot and we aren’t sure if that is because he is a newborn or because of his heart. He also has feeding issues still but again it might just be due to everything he has been through and not because of his heart. The question is – although his heartrate is low, is it steady and stable enough to delay installing a pacemaker until his 2nd surgery? There are risks and benefits to both situations. If they decide to put it in now, the same incision on his chest will have to be opened as well as a new one on his belly. He’ll have to go back on the ventilator, stay at least overnight in the ICU, and then we would have to work on his feedings all over again. If there is room, he could have the surgery on Friday, otherwise have it on Monday. I would guess we’d be here through the end of next week.
If they decide to hold off, we can essentially leave. It is the only thing holding us here. He doesn’t eat well so we need to learn how to take care of his NG tube. I installed the one he is using now and it did stink to have him cry so much but it really wasn’t that big of a deal. We can work on his feedings at home just as well (or better) than at the hospital. We would just need to watch him more carefully and they would teach us those signs. All he needs is his “little boy” procedure and we could go. Holy cow. They would make sure we are well educated before going home.
Evan is also no longer considered to be in complete heart block (3rd degree heart block). They said he is more into a 2nd degree heart block with his atrium conduction followed by the ventricles, but that there is a pattern of a growing delay between those two events. I checked it out and it sounds like Type 1 (Mobitz I/Wenckebach). Here is another source. When we were discussing his condition the nurse was watching his ECG and noticed that Evan had 4 normal heart beats in a row. So maybe he will be ok after all. That’s why they are going to look at the past 24 hours worth of data and also why they get paid the big bucks to make decisions like these.
I understand better now where the debate was and why they wanted us to wait so long. I don’t really know how to feel or what to think; I would just be nervous without one but the thought of him not having to undergo another procedure at this point is very appealing. Just the thought of being able to have a cordless baby makes me giddy with excitement.